The effect of bevacizumab on corneal neovascularization in rabbits
- PMID: 20714387
- PMCID: PMC2916105
- DOI: 10.3341/kjo.2010.24.4.230
The effect of bevacizumab on corneal neovascularization in rabbits
Abstract
Purpose: To determine the efficacy of topical application and subconjunctival injection of bevacizumab in the treatment of corneal neovascularization.
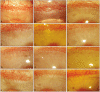
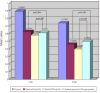
Methods: Corneal neovascularization was induced with a silk suture of the corneal stroma in 12 rabbits (24 eyes). One week after suturing, four rabbits were treated with topical bevacizumab at 5 mg/mL (group A) and another four rabbits were treated with topical bevacizumab 10 mg/mL (group B) in the right eyes twice a day for two weeks. A subconjunctival injection of bevacizumab 1.25 mg/mL was done in the right eyes of four rabbits (group C). All of the left eyes (12 eyes) were used as controls. The area of corneal neovascularization was measured after one and two weeks, and the concentration of vascular endothelial growth factor (VEGF) in corneal tissue was measured after two weeks.
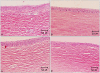
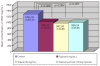
Results: The neovascularized area was smaller in all treated groups than in the control group (p<0.001). Upon analysis of the neovascularized area, there was no significant difference between groups A and B. However, the mean neovascularized area of group B was significantly smaller than that of group C after two weeks of treatment (p=0.043). The histologic examination revealed fewer new corneal vessels in all treated groups than the control group. The concentration of VEGF was significantly lower in all treated groups compared to the control group (p<0.01), but no difference was shown between treated groups.
Conclusions: Topical and subconjunctival bevacizumab application may be useful in the treatment of corneal neovascularization and further study is necessary.
Keywords: Bevacizumab; Cornea; Neovascularization.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
Similar articles
-
The effect of subconjunctival suramin on corneal neovascularization in rabbits.Cornea. 2010 Jan;29(1):86-92. doi: 10.1097/ICO.0b013e3181ae91e3. Cornea. 2010. PMID: 19907290
-
Inhibition of experimental corneal neovascularization by using subconjunctival injection of bevacizumab (Avastin).Cornea. 2008 Apr;27(3):349-52. doi: 10.1097/ICO.0b013e31815cf67d. Cornea. 2008. PMID: 18362666
-
Inhibition of corneal neovascularization by subconjunctival and topical bevacizumab and sunitinib in a rabbit model.Cornea. 2013 May;32(5):689-95. doi: 10.1097/ICO.0b013e3182801645. Cornea. 2013. PMID: 23377751
-
Corneal neovascularization and the utility of topical VEGF inhibition: ranibizumab (Lucentis) vs bevacizumab (Avastin).Ocul Surf. 2012 Apr;10(2):67-83. doi: 10.1016/j.jtos.2012.01.005. Epub 2012 Jan 25. Ocul Surf. 2012. PMID: 22482468 Free PMC article. Review.
-
Corneal neovascularization: an anti-VEGF therapy review.Surv Ophthalmol. 2012 Sep;57(5):415-29. doi: 10.1016/j.survophthal.2012.01.007. Surv Ophthalmol. 2012. PMID: 22898649 Free PMC article. Review.
Cited by
-
Ocular delivery of macromolecules.J Control Release. 2014 Sep 28;190:172-81. doi: 10.1016/j.jconrel.2014.06.043. Epub 2014 Jul 3. J Control Release. 2014. PMID: 24998941 Free PMC article. Review.
-
The toxicity of intrathecal bevacizumab in a rabbit model of leptomeningeal carcinomatosis.J Neurooncol. 2012 Jan;106(1):81-8. doi: 10.1007/s11060-011-0655-9. Epub 2011 Jul 26. J Neurooncol. 2012. PMID: 21789699
-
Resolution of Refractory Corneal Neovascularization with Subconjunctival Bevacizumab.Case Rep Ophthalmol. 2020 Dec 7;11(3):652-657. doi: 10.1159/000510114. eCollection 2020 Sep-Dec. Case Rep Ophthalmol. 2020. PMID: 33442379 Free PMC article.
-
Inhibitory Effect of Topical Cartilage Acellular Matrix Suspension Treatment on Neovascularization in a Rabbit Corneal Model.Tissue Eng Regen Med. 2020 Oct;17(5):625-640. doi: 10.1007/s13770-020-00275-3. Epub 2020 Jul 2. Tissue Eng Regen Med. 2020. PMID: 32617955 Free PMC article.
-
Transplantation of PEDF-transfected pigment epithelial cells inhibits corneal neovascularization in a rabbit model.Graefes Arch Clin Exp Ophthalmol. 2015 Jul;253(7):1061-9. doi: 10.1007/s00417-015-2954-x. Epub 2015 Feb 18. Graefes Arch Clin Exp Ophthalmol. 2015. PMID: 25690979
References
-
- Dana MR, Streilein JW. Loss and restoration of immune privilege in eyes with corneal neovascularization. Invest Ophthalmol Vis Sci. 1996;37:2485–2494. - PubMed
-
- Lee P, Wang CC, Adamis AP. Ocular neovascularization: an epidemiologic review. Surv Ophthalmol. 1998;43:245–269. - PubMed
-
- Riazi-Esfahani M, Peyman GA, Aydin E, et al. Prevention of corneal neovascularization: evaluation of various commercially available compounds in an experimental rat model. Cornea. 2006;25:801–805. - PubMed
-
- Ambati BK, Joussen AM, Ambati J, et al. Angiostatin inhibits and regresses corneal neovascularization. Arch Ophthalmol. 2002;120:1063–1068. - PubMed
-
- Shao C, Sima J, Zhang SX, et al. Suppression of corneal neovascularization by PEDF release from human amniotic membranes. Invest Ophthalmol Vis Sci. 2004;45:1758–1762. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

