Sympathetic nerve-dependent regulation of mucosal vascular tone modifies airway smooth muscle reactivity
- PMID: 20724568
- PMCID: PMC2980371
- DOI: 10.1152/japplphysiol.00632.2010
Sympathetic nerve-dependent regulation of mucosal vascular tone modifies airway smooth muscle reactivity
Abstract
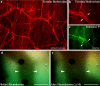
The airways contain a dense subepithelial microvascular plexus that is involved in the supply and clearance of substances to and from the airway wall. We set out to test the hypothesis that airway smooth muscle reactivity to bronchoconstricting agents may be dependent on airway mucosal blood flow. Immunohistochemical staining identified vasoconstrictor and vasodilator nerve fibers associated with subepithelial blood vessels in the guinea pig airways. Intravital microscopy of the tracheal mucosal microvasculature in anesthetized guinea pigs revealed that blockade of α-adrenergic receptors increased baseline arteriole diameter by ~40%, whereas the α-adrenergic receptor agonist phenylephrine produced a modest (5%) vasoconstriction in excess of the baseline tone. In subsequent in vivo experiments, tracheal contractions evoked by topically applied histamine were significantly reduced (P < 0.05) and enhanced by α-adrenergic receptor blockade and activation, respectively. α-Adrenergic ligands produced similar significant (P < 0.05) effects on airway smooth muscle contractions evoked by topically administered capsaicin, intravenously administered neurokinin A, inhaled histamine, and topically administered antigen in sensitized animals. These responses were independent of any direct effect of α-adrenergic ligands on the airway smooth muscle tone. The data suggest that changes in blood flow in the vessels supplying the airways regulate the reactivity of the underlying airway smooth muscle to locally released and exogenously administered agents by regulating their clearance. We speculate that changes in mucosal vascular function or changes in neuronal regulation of the airway vasculature may contribute to airways responsiveness in disease.
Figures


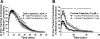

Comment in
-
Microvascular blood flow in the airway mucosa modulates bronchoconstriction.J Appl Physiol (1985). 2010 Nov;109(5):1287. doi: 10.1152/japplphysiol.01079.2010. Epub 2010 Sep 16. J Appl Physiol (1985). 2010. PMID: 20847125 No abstract available.
Similar articles
-
Microvascular blood flow in the airway mucosa modulates bronchoconstriction.J Appl Physiol (1985). 2010 Nov;109(5):1287. doi: 10.1152/japplphysiol.01079.2010. Epub 2010 Sep 16. J Appl Physiol (1985). 2010. PMID: 20847125 No abstract available.
-
The non-adrenergic, non-cholinergic response counteracts changes in guinea-pig airway tone with and without sympathetic activation.Br J Pharmacol. 1992 Jul;106(3):616-22. doi: 10.1111/j.1476-5381.1992.tb14384.x. Br J Pharmacol. 1992. PMID: 1354543 Free PMC article.
-
Reflex regulation of airway sympathetic nerves in guinea-pigs.J Physiol. 2006 Jun 1;573(Pt 2):549-64. doi: 10.1113/jphysiol.2005.104661. Epub 2006 Mar 31. J Physiol. 2006. PMID: 16581869 Free PMC article.
-
Cholinergic and neurogenic mechanisms in obstructive airways disease.Am J Med. 1986 Nov 14;81(5A):93-102. doi: 10.1016/0002-9343(86)90470-5. Am J Med. 1986. PMID: 2878614 Review.
-
Innervation of airway smooth muscle. Efferent mechanisms.Pharmacol Ther. 1987;32(2):107-30. doi: 10.1016/0163-7258(87)90055-6. Pharmacol Ther. 1987. PMID: 2885861 Review.
Cited by
-
Molecular identity, anatomy, gene expression and function of neural crest vs. placode-derived nociceptors in the lower airways.Neurosci Lett. 2021 Jan 18;742:135505. doi: 10.1016/j.neulet.2020.135505. Epub 2020 Nov 13. Neurosci Lett. 2021. PMID: 33197519 Free PMC article. Review.
-
Vagal Afferent Innervation of the Airways in Health and Disease.Physiol Rev. 2016 Jul;96(3):975-1024. doi: 10.1152/physrev.00039.2015. Physiol Rev. 2016. PMID: 27279650 Free PMC article. Review.
-
Neuronal modulation of airway and vascular tone and their influence on nonspecific airways responsiveness in asthma.J Allergy (Cairo). 2012;2012:108149. doi: 10.1155/2012/108149. Epub 2012 Oct 23. J Allergy (Cairo). 2012. PMID: 23150736 Free PMC article.
-
Investigation of vagal sensory neurons in mice using optical vagal stimulation and tracheal neuroanatomy.iScience. 2024 Feb 9;27(3):109182. doi: 10.1016/j.isci.2024.109182. eCollection 2024 Mar 15. iScience. 2024. PMID: 38414860 Free PMC article.
-
Structure of vagal afferent nerve terminal fibers in the mouse trachea.Respir Physiol Neurobiol. 2018 Feb;249:35-46. doi: 10.1016/j.resp.2018.01.001. Epub 2018 Jan 4. Respir Physiol Neurobiol. 2018. PMID: 29306061 Free PMC article.
References
-
- Bai TR, Lam R, Prasad FY. Effects of adrenergic agonists and adenosine on cholinergic neurotransmission in human tracheal smooth muscle. Pulm Pharmacol 1: 193–199, 1989 - PubMed
-
- Bianco S, Pieroni MG, Refini RM, Rottoli L, Sestini P. Protective effect of inhaled furosemide on allergen-induced early and late asthmatic reactions. N Engl J Med 321: 1069–1073, 1989 - PubMed
-
- Brieva J, Wanner A. Adrenergic airway vascular smooth muscle responsiveness in healthy and asthmatic subjects. J Appl Physiol 90: 665–669, 2001 - PubMed
-
- Brown DL, Guyenet PG. Electrophysiological study of cardiovascular neurons in the rostral ventrolateral medulla in rats. Circ Res 56: 359–369, 1985 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

