Bench-to-bedside review: Glucose and stress conditions in the intensive care unit
- PMID: 20727232
- PMCID: PMC2945096
- DOI: 10.1186/cc9100
Bench-to-bedside review: Glucose and stress conditions in the intensive care unit
Abstract
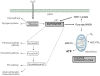
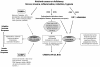
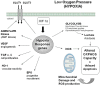
The physiological response to blood glucose elevation is the pancreatic release of insulin, which blocks hepatic glucose production and release, and stimulates glucose uptake and storage in insulin-dependent tissues. When this first regulatory level is overwhelmed (that is, by exogenous glucose supplementation), persistent hyperglycaemia occurs with intricate consequences related to the glucose acting as a metabolic substrate and as an intracellular mediator. It is thus very important to unravel the glucose metabolic pathways that come into play during stress as well as the consequences of these on cellular functions. During acute injuries, activation of serial hormonal and humoral responses inducing hyperglycaemia is called the 'stress response'. Central activation of the nervous system and of the neuroendocrine axes is involved, releasing hormones that in most cases act to worsen the hyperglycaemia. These hormones in turn induce profound modifications of the inflammatory response, such as cytokine and mediator profiles. The hallmarks of stress-induced hyperglycaemia include 'insulin resistance' associated with an increase in hepatic glucose output and insufficient release of insulin with regard to glycaemia. Although both acute and chronic hyperglycaemia may induce deleterious effects on cells and organs, the initial acute endogenous hyperglycaemia appears to be adaptive. This acute hyperglycaemia participates in the maintenance of an adequate inflammatory response and consequently should not be treated aggressively. Hyperglycaemia induced by an exogenous glucose supply may, in turn, amplify the inflammatory response such that it becomes a disproportionate response. Since chronic exposure to glucose metabolites, as encountered in diabetes, induces adverse effects, the proper roles of these metabolites during acute conditions need further elucidation.
Figures

References
-
- Hotamisligil GS. Inflammation and metabolic disorders. Nature. 2006;444:860–867. - PubMed
-
- Bernard C. Leçon sur les Phénomènes de la Vie Communs aux Animaux et aux Végétaux. Paris, France: JB Bailliere et Fils; 1877.
-
- Capes SE, Hunt D, Malmberg K, Gerstein HC. Stress hyperglycaemia and increased risk of death after myocardial infarction in patients with and without diabetes: a systematic overview. Lancet. 2000;355:773–778. - PubMed
-
- Van den Berghe G. Molecular biology: a timely tool for further unraveling the "diabetes of stress". Crit Care Med. 2001;29:910–911. - PubMed
-
- Laird AM, Miller PR, Kilgo PD, Meredith JW, Chang MC. Relationship of early hyperglycemia to mortality in trauma patients. J Trauma. 2004;56:1058–1062. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

