Application of an optical clearing agent during noninvasive laser coagulation of the canine vas deferens
- PMID: 20799844
- PMCID: PMC2921419
- DOI: 10.1117/1.3463009
Application of an optical clearing agent during noninvasive laser coagulation of the canine vas deferens
Abstract
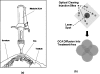
Development of a noninvasive vasectomy technique may eliminate male fear of complications and result in a more popular procedure. This study explores application of an optical clearing agent (OCA) to scrotal skin to reduce laser power necessary for successful noninvasive laser vasectomy and eliminate scrotal skin burns. A mixture of dimethyl sulfoxide and glycerol was noninvasively delivered into scrotal skin using a pneumatic jet device. Near-infrared laser radiation was delivered in conjunction with cryogen spray cooling to the skin surface in a canine model, ex vivo and in vivo. Burst pressure (BP) measurements were conducted to quantify strength of vas closure. A 30-min application of OCA improved skin transparency by 26+/-3%, reducing average power necessary for successful noninvasive laser vasectomy from 9.2 W without OCA (BP=291+/-31 mmHg) to 7.0 W with OCA (BP=292+/-19 mmHg). Control studies without OCA at 7.0 W failed to coagulate the vas with burst pressures (82+/-28 mmHg) significantly below typical ejaculation pressures (136+/-29 mmHg). Application of an OCA reduced the laser power necessary for successful noninvasive thermal coagulation of the vas by approximately 25%. This technique may result in use of a less expensive laser and eliminate the formation of scrotal skin burns during the procedure.
Figures




Similar articles
-
Noninvasive laser coagulation of the human vas deferens: optical and thermal simulations.Lasers Surg Med. 2011 Jul;43(5):443-9. doi: 10.1002/lsm.21057. Lasers Surg Med. 2011. PMID: 21674549
-
High-frequency ultrasound imaging of noninvasive laser coagulation of the canine vas deferens.Lasers Surg Med. 2011 Sep;43(8):838-42. doi: 10.1002/lsm.21098. Lasers Surg Med. 2011. PMID: 21956632 Free PMC article.
-
Noninvasive laser vasectomy: preliminary ex vivo tissue studies.Lasers Surg Med. 2009 Mar;41(3):203-7. doi: 10.1002/lsm.20744. Lasers Surg Med. 2009. PMID: 19291751
-
[Vasectomy and vas deferens contraceptive surgery: legal and technical aspects].Prog Urol. 2007 Jun;17(4):789-93. doi: 10.1016/s1166-7087(07)92293-9. Prog Urol. 2007. PMID: 17633987 Review. French.
-
Vas deferens occlusion during no-scalpel vasectomy.J Fam Pract. 1994 Dec;39(6):577-82. J Fam Pract. 1994. PMID: 7798862 Review.
Cited by
-
Desexing Dogs: A Review of the Current Literature.Animals (Basel). 2019 Dec 5;9(12):1086. doi: 10.3390/ani9121086. Animals (Basel). 2019. PMID: 31817504 Free PMC article. Review.
-
Recent progress in tissue optical clearing.Laser Photon Rev. 2013 Sep;7(5):732-757. doi: 10.1002/lpor.201200056. Epub 2013 Feb 5. Laser Photon Rev. 2013. PMID: 24348874 Free PMC article.
-
In vivo skin optical clearing for improving imaging and light-induced therapy: a review.J Biomed Opt. 2023 Jun;28(6):060901. doi: 10.1117/1.JBO.28.6.060901. Epub 2023 Jun 6. J Biomed Opt. 2023. PMID: 37288448 Free PMC article. Review.
-
Optical clearing of vaginal tissues, ex vivo, for minimally invasive laser treatment of female stress urinary incontinence.J Biomed Opt. 2017 Jan 1;22(1):18002. doi: 10.1117/1.JBO.22.1.018002. J Biomed Opt. 2017. PMID: 28301637 Free PMC article.
-
Vasectomy techniques--need for better occlusion methods.Asian J Androl. 2010 May;12(3):442-3. doi: 10.1038/aja.2010.10. Epub 2010 Mar 15. Asian J Androl. 2010. PMID: 20228824 Free PMC article. No abstract available.
References
-
- Mosher W. D., Martinez G. M., Chandra A., Abma J. C., and Wilson S. J., “Use of contraception and use of family planning services in the United States: 1982–2002,” Adv. Data 350, 1–36 (2004). - PubMed
-
- Chandra A., Martinez G. M., Mosher W. D., Abma J. C., and Jones C., “Fertility, family planning, and reproductive health of U.S. women: data from the 2002 National Survey of Family Growth,” Vital Health Stat. 25, 1–160 (2005). - PubMed
-
- Martinez G. M., Chandra A., Abma J. C., Jones J., and Mosher W. D., “Fertility, contraception, and fatherhood: data on men and women from cycle 6 (2002) of the 2002 National Survey of Family Growth,” Vital Health Stat. 26, 1–142 (2006). - PubMed
-
- Miller W. B., Shain R. N., and Pasta D. J., “Tubal sterilization or vasectomy: how do married couples make the choice,” Fertil. Steril. FESTAS 56, 278–284 (1991). - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

