Atopic asthmatic subjects but not atopic subjects without asthma have enhanced inflammatory response to ozone
- PMID: 20816188
- PMCID: PMC2949284
- DOI: 10.1016/j.jaci.2010.06.043
Atopic asthmatic subjects but not atopic subjects without asthma have enhanced inflammatory response to ozone
Abstract
Background: Asthma is a known risk factor for acute ozone-associated respiratory disease. Ozone causes an immediate decrease in lung function and increased airway inflammation. The role of atopy and asthma in modulation of ozone-induced inflammation has not been determined.
Objective: We sought to determine whether atopic status modulates ozone response phenotypes in human subjects.
Methods: Fifty volunteers (25 healthy volunteers, 14 atopic nonasthmatic subjects, and 11 atopic asthmatic subjects not requiring maintenance therapy) underwent a 0.4-ppm ozone exposure protocol. Ozone response was determined based on changes in lung function and induced sputum composition, including airway inflammatory cell concentration, cell-surface markers, and cytokine and hyaluronic acid concentrations.
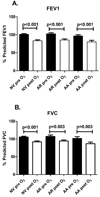
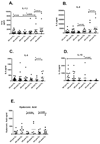
Results: All cohorts experienced similar decreases in lung function after ozone. Atopic and atopic asthmatic subjects had increased sputum neutrophil numbers and IL-8 levels after ozone exposure; values did not significantly change in healthy volunteers. After ozone exposure, atopic asthmatic subjects had significantly increased sputum IL-6 and IL-1beta levels and airway macrophage Toll-like receptor 4, Fc(epsilon)RI, and CD23 expression; values in healthy volunteers and atopic nonasthmatic subjects showed no significant change. Atopic asthmatic subjects had significantly decreased IL-10 levels at baseline compared with healthy volunteers; IL-10 levels did not significantly change in any group with ozone. All groups had similar levels of hyaluronic acid at baseline, with increased levels after ozone exposure in atopic and atopic asthmatic subjects.
Conclusion: Atopic asthmatic subjects have increased airway inflammatory responses to ozone. Increased Toll-like receptor 4 expression suggests a potential pathway through which ozone generates the inflammatory response in allergic asthmatic subjects but not in atopic subjects without asthma.
Published by Mosby, Inc.
Conflict of interest statement
Disclosure of potential conflict of interest: B. Harris has received research support from the National Institute of Environmental Health Sciences, the US Environmental Protection Agency, and Purdue Pharmaceuticals–Quintiles. P. A. Bromberg has received research support from the US Environmental Protection Agency and the National Institutes of Health. D. B. Peden has consulted for GlaxoSmithKline and Funxional Therapeutics and has received research support from the National Institute of Environmental Health Sciences; the National Institute for Allergy and Infectious Diseases; the National Center for Complementary and Alternative Medicine; the National Heart, Lung, and Blood Institute; the US Environmental Protection Agency; the National Center for Research Resources. The rest of the authors have declared that they have no conflict of interest.
Figures


Similar articles
-
Airway purinergic responses in healthy, atopic nonasthmatic, and atopic asthmatic subjects exposed to ozone.Inhal Toxicol. 2011 May;23(6):324-30. doi: 10.3109/08958378.2011.572096. Inhal Toxicol. 2011. PMID: 21605007 Free PMC article.
-
Differential regulation of allergen-specific T(H2)- but not T(H1)-type responses by alveolar macrophages in atopic asthma.J Allergy Clin Immunol. 1998 Sep;102(3):368-75. doi: 10.1016/s0091-6749(98)70122-8. J Allergy Clin Immunol. 1998. PMID: 9768575
-
Effect of ozone and nitrogen dioxide on the release of proinflammatory mediators from bronchial epithelial cells of nonatopic nonasthmatic subjects and atopic asthmatic patients in vitro.J Allergy Clin Immunol. 2001 Feb;107(2):287-94. doi: 10.1067/mai.2001.111141. J Allergy Clin Immunol. 2001. PMID: 11174195
-
Atopic asthmatic patients have reduced airway inflammatory cell recruitment after inhaled endotoxin challenge compared with healthy volunteers.J Allergy Clin Immunol. 2012 Oct;130(4):869-76.e2. doi: 10.1016/j.jaci.2012.05.026. Epub 2012 Jul 4. J Allergy Clin Immunol. 2012. PMID: 22770265 Free PMC article.
-
Rhinovirus-Induced Cytokine Alterations With Potential Implications in Asthma Exacerbations: A Systematic Review and Meta-Analysis.Front Immunol. 2022 Feb 15;13:782936. doi: 10.3389/fimmu.2022.782936. eCollection 2022. Front Immunol. 2022. PMID: 35242128 Free PMC article.
Cited by
-
Ozone-Induced Oxidative Stress, Neutrophilic Airway Inflammation, and Glucocorticoid Resistance in Asthma.Front Immunol. 2021 Feb 26;12:631092. doi: 10.3389/fimmu.2021.631092. eCollection 2021. Front Immunol. 2021. PMID: 33717165 Free PMC article. Review.
-
Protective Role of Eosinophils and TNFa after Ozone Inhalation.Res Rep Health Eff Inst. 2017 Mar;2017(191):1-41. Res Rep Health Eff Inst. 2017. PMID: 29659241 Free PMC article.
-
Airway purinergic responses in healthy, atopic nonasthmatic, and atopic asthmatic subjects exposed to ozone.Inhal Toxicol. 2011 May;23(6):324-30. doi: 10.3109/08958378.2011.572096. Inhal Toxicol. 2011. PMID: 21605007 Free PMC article.
-
The effect of environmental oxidative stress on airway inflammation.Curr Opin Allergy Clin Immunol. 2012 Apr;12(2):133-9. doi: 10.1097/ACI.0b013e32835113d6. Curr Opin Allergy Clin Immunol. 2012. PMID: 22306553 Free PMC article. Review.
-
Exposure to ozone modulates human airway protease/antiprotease balance contributing to increased influenza A infection.PLoS One. 2012;7(4):e35108. doi: 10.1371/journal.pone.0035108. Epub 2012 Apr 9. PLoS One. 2012. PMID: 22496898 Free PMC article.
References
-
- Peden D. Air Pollution: Indoor and Outdoor. In: Adkinson NF Jr, Busse W, Bochner B, Holgate S, Simons FE, Lemanske R, editors. MIDDLETON'S ALLERGY: PRINCIPLES AND PRACTICE. 7 ed ed. Mosby: 2008. pp. 495–508.
-
- Bernstein JA, Alexis N, Barnes C, Bernstein IL, Nel A, Peden D, et al. Health effects of air pollution. J Allergy Clin Immunol. 2004;114:1116–1123. - PubMed
-
- Peden DB. The epidemiology and genetics of asthma risk associated with air pollution. J Allergy Clin Immunol. 2005;115:213–219. quiz 20. - PubMed
-
- Peden DB, Boehlecke B, Horstman D, Devlin R. Prolonged acute exposure to 0.16 ppm ozone induces eosinophilic airway inflammation in asthmatic subjects with allergies. J Allergy Clin Immunol. 1997;100:802–808. - PubMed
-
- Kehrl HR, Peden DB, Ball B, Folinsbee LJ, Horstman D. Increased specific airway reactivity of persons with mild allergic asthma after 7.6 hours of exposure to 0.16 ppm ozone. J Allergy Clin Immunol. 1999;104:1198–1204. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- R01ES012706/ES/NIEHS NIH HHS/United States
- M01RR00046/RR/NCRR NIH HHS/United States
- P01AT002620/AT/NCCIH NIH HHS/United States
- U19 AI077437/AI/NIAID NIH HHS/United States
- P01 AT002620/AT/NCCIH NIH HHS/United States
- KL2 RR025746/RR/NCRR NIH HHS/United States
- KL2RR025746/RR/NCRR NIH HHS/United States
- P30 ES010126/ES/NIEHS NIH HHS/United States
- M01 RR000046/RR/NCRR NIH HHS/United States
- R01 ES012706/ES/NIEHS NIH HHS/United States
- UL1RR025747/RR/NCRR NIH HHS/United States
- UL1 RR025747/RR/NCRR NIH HHS/United States
- U19AI077437/AI/NIAID NIH HHS/United States
- P30ES010126/ES/NIEHS NIH HHS/United States

