Incidence and reasons for nonrevision reoperation after total knee arthroplasty
- PMID: 20848243
- PMCID: PMC3008870
- DOI: 10.1007/s11999-010-1558-3
Incidence and reasons for nonrevision reoperation after total knee arthroplasty
Abstract
Background: A dramatic increase in the demand for TKA is expected. The current burden of revision TKA is well known but the incidence and etiology of nonrevision reoperations after primary TKA is not.
Questions/purposes: We determined the rate, reason, timing, and predictors of nonrevision reoperation after TKA.
Methods: Using our institutional joint arthroplasty database, we identified 10,188 TKA performed on 7,613 patients between April 2000 and March 2008. A nonrevision reoperation was defined as any procedure requiring anesthetic in which components with bony interfaces were not removed or exchanged. Procedures after revision TKA were excluded. Potential risk factors investigated included age, gender, laterality, and simultaneous bilateral versus staged bilateral versus unilateral TKA. The minimum followup was 1 year (median, 4.1 years; range, 1.1 to 9.1 years).
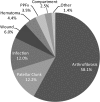
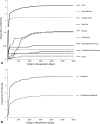
Results: Three hundred fifty-three patients of 7,613 (4.6%) underwent 434 nonrevision reoperations on 384 of 10,188 (3.8%) knees. The most common indication for nonrevision reoperation was stiffness (58%; 252 of 434), followed by patellar clunk (12%; 53), infection (12%; 52), wound revision (6%; 26), hematoma (4.4%; 19), among others. The median time to reoperation was 74.5 days (range, 1-3058 days) but varied widely. Younger patients and those with unilateral TKA were more likely to have a nonrevision reoperation.
Conclusions: The majority of nonrevision reoperations are performed for stiffness. Patellar clunk and infection also result in a large number of nonrevision reoperations. In weighing the future economic and workforce burden of TKA, nonrevision reoperations need to be acknowledged, and preventive measures need to be implemented.
Level of evidence: Level II, prognostic study. See the Guidelines for Authors for a complete description of levels of evidence.
Figures
References
-
- Hartman MB, Fehring TK, Jordan L, Norton HJ. Periprosthetic knee sepsis. The role of irrigation and debridement. Clin Orthop Relat Res. 1991;273:113–118. - PubMed
-
- Hozack WJ, Rothman RH, Booth RE, Jr, Balderston RA. The patellar clunk syndrome. A complication of posterior stabilized total knee arthroplasty. Clin Orthop Relat Res. 1989;241:203–208. - PubMed
-
- Iorio R, Robb WJ, Healy WL, Berry DJ, Hozack WJ, Kyle RF, Lewallen DG, Trousdale RT, Jiranek WA, Stamos VP, Parsley BS. Orthopaedic surgeon workforce and volume assessment for total hip and knee replacement in the United States: preparing for an epidemic. J Bone Joint Surg Am. 2008;90:1598–1605. doi: 10.2106/JBJS.H.00067. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous