Intraoperative spinal cord and nerve root monitoring: a survey of Canadian spine surgeons
- PMID: 20858377
- PMCID: PMC2947118
Intraoperative spinal cord and nerve root monitoring: a survey of Canadian spine surgeons
Abstract
Background: Intraoperative spinal cord and nerve root monitoring is used to identify an insult to the neural elements with the goal of preventing injury. There are 2 major categories of monitoring: evoked potentials (somatosensory evoked potentials and motor evoked potentials) and electromyography. The availability of intraoperative neuromonitoring and the indications for use vary widely. In this study, we aimed to document the current practices and opinions of Canadian spine surgeons with regards to intraoperative spinal monitoring.
Methods: We surveyed members of the Canadian Spine Society about the availability and use of various types of intraoperative neuromonitoring modalities for surgical procedures.
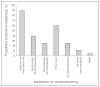
Results: We distributed 105 surveys and received 95 responses (90%). Somatosensory evoked potentials were the most commonly available form of intraoperative neuromonitoring, although it was available to only 65.3% of respondents. Surgeons in either full-time or part-time academic practice used monitoring more frequently than those in private practice (p < 0.001), but this association was not based on surgeon preference after controlling for availability. Years of practice and training background (orthopedic or neurosurgical) did not influence the use of monitoring. Canadian spine surgeons overwhelmingly reported that they use intraoperative neuromonitoring to reduce the risk of adverse operative events, rather than because of liability concerns. Most respondents believed that monitoring should be used in the correction of major deformity and scoliosis.
Conclusion: The availability of spinal monitoring in Canada is variable. Most surgeons believe that it is an important adjunct to improve patient safety.
Contexte: La surveillance intraopératoire de la moelle épinière et des racines nerveuses sert à déterminer l’atteinte des éléments nerveux afin de prévenir des lésions. Il y a 2 grandes catégories de surveillance: les potentiels évoqués (potentiels évoqués somatosensoriels et potentiels évoqués moteurs) et l’électromyographie. La disponibilité de la neurosurveillance intraopératoire et les indications de son utilisation varient énormément. Au cours de cette étude, nous voulions documenter les pratiques et les opinions courantes des chirurgiens canadiens spécialistes du rachis en ce qui a trait à la surveillance intraopératoire de la moelle.
Méthodes: Nous avons sondé les membres de la Société canadienne du rachis au sujet de la disponibilité et de l’utilisation de diverses méthodes de neurosurveillance intraopératoire durant les interventions chirurgicales.
Résultats: Nous avons distribué 105 questionnaires et reçu 95 réponses (90 %). Les potentiels évoqués somatosensoriels constituaient la forme la plus répandue de neurosurveillance intraopératoire, même si 65,3 % seulement des répondants y avaient accès. Les chirurgiens de pratique universitaire à temps plein ou à temps partiel utilisaient la surveillance plus souvent que ceux qui exerçaient en pratique privée (p < 0,001), mais ce lien n’était pas basé sur la préférence du chirurgien compte tenu de la disponibilité. Le nombre d’années de pratique et la formation (en orthopédie ou en neurochirurgie) n’avaient pas d’effet sur l’utilisation de la surveillance. Les chirurgiens canadiens spécialistes du rachis ont déclaré par une majorité écrasante qu’ils utilisent la neurosurveillance intraopératoire afin de réduire le risque d’événements indésirables au cours de l’intervention plutôt qu’à cause de préoccupations liées à la responsabilité. La plupart des répondants sont d’avis qu’il faudrait utiliser la surveillance dans les interventions de correction d’une malformation majeure et d’une scoliose.
Conclusion: La disponibilité de la surveillance de la moelle au Canada est variable. La plupart des chirurgiens croient qu’il s’agit d’un outil d’appoint important pour améliorer la sécurité des patients.
Figures
Similar articles
-
Intraoperative Spinal Cord and Nerve Root Monitoring: A Hospital Survey and Review.Bull Hosp Jt Dis (2013). 2015 Mar;73(1):25-36. Bull Hosp Jt Dis (2013). 2015. PMID: 26516998 Review.
-
Neurophysiological detection of impending spinal cord injury during scoliosis surgery.J Bone Joint Surg Am. 2007 Nov;89(11):2440-9. doi: 10.2106/JBJS.F.01476. J Bone Joint Surg Am. 2007. PMID: 17974887
-
Continuous electromyographic monitoring to detect nerve root injury during thoracolumbar scoliosis surgery.Spine (Phila Pa 1976). 1997 Nov 1;22(21):2547-50. doi: 10.1097/00007632-199711010-00016. Spine (Phila Pa 1976). 1997. PMID: 9383863
-
Intraoperative neurophysiologic detection of iatrogenic C5 nerve root injury during laminectomy for cervical compression myelopathy.Spine (Phila Pa 1976). 2002 Nov 15;27(22):2499-502. doi: 10.1097/00007632-200211150-00014. Spine (Phila Pa 1976). 2002. PMID: 12435981 Clinical Trial.
-
Intraoperative neurophysiological monitoring during spine surgery: a review.Neurosurg Focus. 2009 Oct;27(4):E6. doi: 10.3171/2009.8.FOCUS09150. Neurosurg Focus. 2009. PMID: 19795955 Review.
Cited by
-
Interpretation of surgical neuromonitoring data in Canada: a survey of practising surgeons.Can J Surg. 2015 Jun;58(3):206-8. doi: 10.1503/cjs.013214. Can J Surg. 2015. PMID: 25799133 Free PMC article.
-
Intraoperative neuro-monitoring corner editorial: The need for preoperative sep and mep baselines in spinal surgery: Why can't we and our monitoring colleagues get this right?Surg Neurol Int. 2014 Dec 30;5(Suppl 15):S548-51. doi: 10.4103/2152-7806.148036. eCollection 2014. Surg Neurol Int. 2014. PMID: 25593775 Free PMC article.
-
One Approach Anterior Decompression and Fixation with Posterior Unilateral Pedicle Screw Fixation for Thoracolumbar Osteoporotic Vertebral Compression Fractures.Orthop Surg. 2021 May;13(3):908-919. doi: 10.1111/os.12947. Epub 2021 Mar 30. Orthop Surg. 2021. PMID: 33787067 Free PMC article.
-
Regional hypothermia inhibits spinal cord somatosensory-evoked potentials without neural damage in uninjured rats.J Neurotrauma. 2013 Aug 1;30(15):1325-33. doi: 10.1089/neu.2012.2516. Epub 2013 Jul 16. J Neurotrauma. 2013. PMID: 22916828 Free PMC article.
-
Estimating Intraoperative Neurophysiological Monitoring Rates for Anterior Cervical Discectomy and Fusion: Are Diagnostic or Procedural Codes Accurate?Int J Spine Surg. 2022 Apr;16(2):208-214. doi: 10.14444/8205. Int J Spine Surg. 2022. PMID: 35444031 Free PMC article.
References
-
- Delank KS, Delank HW, Konig DP, et al. Iatrogenic paraplegia in spinal surgery. Arch Orthop Trauma Surg. 2005;125:33–41. - PubMed
-
- Dawson EG, Sherman JE, Kanim LE, et al. Spinal cord monitoring. Results of the Scoliosis Research Society and the European Spinal Deformity Society survey. Spine. 1991;16:S361–4. - PubMed
-
- Costa P, Bruno A, Bonzanino M, et al. Somatosensory- and motor-evoked potential monitoring during spine and spinal cord surgery. Spinal Cord. 2007;45:86–91. - PubMed
-
- Nuwer MR, Dawson EG, Carlson LG, et al. Somatosensory evoked potential spinal cord monitoring reduces neurologic deficits after scoliosis surgery: results of a large multicenter survey. Electroencephalogr Clin Neurophysiol. 1995;96:6–11. - PubMed
-
- Schwartz DM, Auerbach JD, Dormans JP, et al. Neurophysiological detection of impending spinal cord injury during scoliosis surgery. J Bone Joint Surg Am. 2007;89:2440–9. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources