Predictors of hospital readmission after stroke: a systematic review
- PMID: 20930150
- PMCID: PMC3021413
- DOI: 10.1161/STROKEAHA.110.599159
Predictors of hospital readmission after stroke: a systematic review
Abstract
Background and purpose: Risk-standardized hospital readmission rates are used as publicly reported measures reflecting quality of care. Valid risk-standardized models adjust for differences in patient-level factors across hospitals. We conducted a systematic review of peer-reviewed literature to identify models that compare hospital-level poststroke readmission rates, evaluate patient-level risk scores predicting readmission, or describe patient and process-of-care predictors of readmission after stroke.
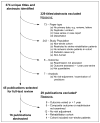
Methods: Relevant studies in English published from January 1989 to July 2010 were identified using MEDLINE, PubMed, Scopus, PsycINFO, and all Ovid Evidence-Based Medicine Reviews. Authors of eligible publications reported readmission within 1 year after stroke hospitalization and identified ≥ 1 predictors of readmission in risk-adjusted statistical models. Publications were excluded if they lacked primary data or quantitative outcomes, reported only composite outcomes, or had < 100 patients.
Results: Of 374 identified publications, 16 met the inclusion criteria for this review. No model was specifically designed to compare risk-adjusted readmission rates at the hospital level or calculate scores predicting a patient's risk of readmission. The studies providing multivariable models of patient-level and/or process-of-care factors associated with readmission varied in stroke definitions, data sources, outcomes (all-cause and/or stroke-related readmission), durations of follow-up, and model covariates. Few characteristics were consistently associated with readmission.
Conclusions: This review identified no risk-standardized models for comparing hospital readmission performance or predicting readmission risk after stroke. Patient-level and system-level factors associated with readmission were inconsistent across studies. The current literature provides little guidance for the development of risk-standardized models suitable for the public reporting of hospital-level stroke readmission performance.
Conflict of interest statement
Figures
References
-
- Medicare Payment Advisory Commission. Report to the Congress: Promoting greater efficiency in Medicare. [Accessed February 17, 2010]. Available at: http://www.medpac.gov/documents/jun07_EntireReport.pdf.
-
- Centers for Medicare & Medicaid Services Hospital Pay-for-Performance Workgroup. US Dept of Health and Human Services Medicare hospital value-based purchasing plan development: Issues paper, 1st public listening session. Jan 172007. [Accessed April 5, 2010]. Available at: http://www.cms.gov/acuteinpatientPPS/downloads/hospital_VBP_plan_issues_....
-
- Institute of Medicine. Rewarding Provider Performance: Aligning Incentives in Medicare. Washington, D.C: National Academy Press; 2007.
-
- Keenan PS, Normand S-LT, Lin Z, Drye EE, Bhat KR, Ross JS, Schuur JD, Stauffer BD, Bernheim SM, Epstein AJ, Wang Y, Herrin J, Chen J, Federer JJ, Mattera JA, Wang Y, Krumholz HM. An administrative claims measure suitable for profiling hospital performance on the basis of 30-day all-cause readmission rates among patients with heart failure. Circ Cardiovasc Qual Outcomes. 2008;1:29–37. - PubMed
-
- Krumholz HM, Merrill AR, Schone EM, Schreiner GC, Chen J, Bradley EH, Wang Y, Wang Y, Lin Z, Straube BM, Rapp MT, Normand S-LT, Drye EE. Patterns of hospital performance in acute myocardial infarction and heart failure 30-day mortality and readmission. Circ Cardiovasc Qual Outcomes. 2009;2:407–413. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous