Functional antibodies targeting IsaA of Staphylococcus aureus augment host immune response and open new perspectives for antibacterial therapy
- PMID: 20956605
- PMCID: PMC3019653
- DOI: 10.1128/AAC.01144-10
Functional antibodies targeting IsaA of Staphylococcus aureus augment host immune response and open new perspectives for antibacterial therapy
Abstract
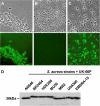
Staphylococcus aureus is the most common cause of nosocomial infections. Multiple antibiotic resistance and severe clinical outcomes provide a strong rationale for development of immunoglobulin-based strategies. Traditionally, novel immunological approaches against bacterial pathogens involve antibodies directed against cell surface-exposed virulence-associated epitopes or toxins. In this study, we generated a monoclonal antibody targeting the housekeeping protein IsaA, a suggested soluble lytic transglycosylase of S. aureus, and tested its therapeutic efficacy in two experimental mouse infection models. A murine anti-IsaA antibody of the IgG1 subclass (UK-66P) showed the highest binding affinity in Biacore analysis. This antibody recognized all S. aureus strains tested, including hospital-acquired and community-acquired methicillin-resistant S. aureus strains. Therapeutic efficacy in vivo in mice was analyzed using a central venous catheter-related infection model and a sepsis survival model. In both models, anti-IsaA IgG1 conferred protection against staphylococcal infection. Ex vivo, UK-66P activates professional phagocytes and induces highly microbicidal reactive oxygen metabolites in a dose-dependent manner, resulting in bacterial killing. The study provides proof of concept that monoclonal IgG1 antibodies with high affinity to the ubiquitously expressed, single-epitope-targeting IsaA are effective in the treatment of staphylococcal infection in different mouse models. Anti-IsaA antibodies might be a useful component in an antibody-based therapeutic for prophylaxis or adjunctive treatment of human cases of S. aureus infections.
Figures

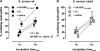


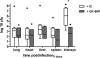

References
-
- Aderem, A. 2003. Phagocytosis and the inflammatory response. J. Infect. Dis. 187(Suppl. 2):S340-S345. - PubMed
-
- Bubeck Wardenburg, J., T. Bae, M. Otto, F. R. Deleo, and O. Schneewind. 2007. Poring over pores: alpha-hemolysin and Panton-Valentine leukocidin in Staphylococcus aureus pneumonia. Nat. Med. 13:1405-1406. - PubMed
-
- Casadevall, A., E. Dadachova, and L. A. Pirofski. 2004. Passive antibody therapy for infectious diseases. Nat. Rev. Microbiol. 2:695-703. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

