Iron and CF-related anemia: expanding clinical and biochemical relationships
- PMID: 20963784
- PMCID: PMC3413076
- DOI: 10.1002/ppul.21335
Iron and CF-related anemia: expanding clinical and biochemical relationships
Abstract
Introduction: This cross-sectional study was conducted to assess the relationship between iron levels in the plasma and sputum of cystic fibrosis (CF) patients.
Methods: Demographic, clinical, and iron-related laboratory data were prospectively obtained from 25 patients with stable clinical features and 14 patients with worsened clinical features since their most recent evaluations.
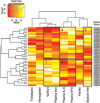
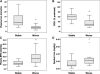
Results: Compared to patients with stable clinical features, those who experienced clinical deterioration demonstrated significantly worse lung function and were more frequently malnourished and diabetic. Members of the latter group were also significantly more hypoferremic and had higher sputum iron content than patients with stable clinical features. No significant correlation was found between plasma and sputum iron levels when the groups were analyzed together and separately.
Conclusions: Sputum iron content does not correlate with iron-related hematologic tests. Hypoferremia is common in CF and correlates with poor lung function and overall health.
Copyright © 2011 Wiley-Liss, Inc.
Figures

Similar articles
-
A pilot study of cystic fibrosis exacerbation response phenotypes reveals contrasting serum and sputum iron trends.Sci Rep. 2021 Mar 1;11(1):4897. doi: 10.1038/s41598-021-84041-y. Sci Rep. 2021. PMID: 33649353 Free PMC article.
-
Iron supplementation does not worsen respiratory health or alter the sputum microbiome in cystic fibrosis.J Cyst Fibros. 2014 May;13(3):311-8. doi: 10.1016/j.jcf.2013.11.004. Epub 2013 Dec 13. J Cyst Fibros. 2014. PMID: 24332997 Free PMC article. Clinical Trial.
-
Iron homeostasis during cystic fibrosis pulmonary exacerbation.Clin Transl Sci. 2012 Aug;5(4):368-73. doi: 10.1111/j.1752-8062.2012.00417.x. Epub 2012 Jun 1. Clin Transl Sci. 2012. PMID: 22883617 Free PMC article. Clinical Trial.
-
Diabetes mellitus in cystic fibrosis.Eur J Gastroenterol Hepatol. 1996 Aug;8(8):744-7. Eur J Gastroenterol Hepatol. 1996. PMID: 8864669 Review.
-
Leukotriene receptor antagonists in children with cystic fibrosis lung disease : anti-inflammatory and clinical effects.Paediatr Drugs. 2005;7(6):353-63. doi: 10.2165/00148581-200507060-00004. Paediatr Drugs. 2005. PMID: 16356023 Review.
Cited by
-
A pilot study of cystic fibrosis exacerbation response phenotypes reveals contrasting serum and sputum iron trends.Sci Rep. 2021 Mar 1;11(1):4897. doi: 10.1038/s41598-021-84041-y. Sci Rep. 2021. PMID: 33649353 Free PMC article.
-
Use of a Multiplex Transcript Method for Analysis of Pseudomonas aeruginosa Gene Expression Profiles in the Cystic Fibrosis Lung.Infect Immun. 2016 Sep 19;84(10):2995-3006. doi: 10.1128/IAI.00437-16. Print 2016 Oct. Infect Immun. 2016. PMID: 27481238 Free PMC article.
-
Iron Deficiency in Cystic Fibrosis: A Cross-Sectional Single-Centre Study in a Referral Adult Centre.Nutrients. 2022 Feb 5;14(3):673. doi: 10.3390/nu14030673. Nutrients. 2022. PMID: 35277032 Free PMC article.
-
Heme protects Pseudomonas aeruginosa and Staphylococcus aureus from calprotectin-induced iron starvation.J Biol Chem. 2021 Jan-Jun;296:100160. doi: 10.1074/jbc.RA120.015975. Epub 2020 Dec 9. J Biol Chem. 2021. PMID: 33273016 Free PMC article.
-
Nitric Oxide and Iron Signaling Cues Have Opposing Effects on Biofilm Development in Pseudomonas aeruginosa.Appl Environ Microbiol. 2019 Jan 23;85(3):e02175-18. doi: 10.1128/AEM.02175-18. Print 2019 Feb 1. Appl Environ Microbiol. 2019. PMID: 30478229 Free PMC article.
References
-
- Strausbaugh SD, Davis PB. Cystic fibrosis: a review of epidemiology and pathobiology. Clin Chest Med. 2007;28:279–288. - PubMed
-
- Rosenfeld M, Ramsey BW, Gibson RL. Pseudomonas acquisition in young patients with cystic fibrosis: pathophysiology, diagnosis, and management. Curr Opin Pulm Med. 2003;9:492–497. - PubMed
-
- Konstan MW, Morgan WJ, Butler SM, Pasta DJ, Craib ML, Silva SJ, Stokes DC, Wohl ME, Wagener JS, Regelmann WE, Johnson CA, the Scientific Advisory Group and the Investigators and Coordinators of the Epidemiologic Study of Cystic Fibrosis Risk factors for rate of decline in forced expiratory volume in one second in children and adolescents with cystic fibrosis. J Pediatr. 2007;151:134–139. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

