Perfusion CT imaging of brain tumors: an overview
- PMID: 21051510
- PMCID: PMC7965371
- DOI: 10.3174/ajnr.A2263
Perfusion CT imaging of brain tumors: an overview
Abstract
Perfusion imaging of brain tumors has been performed by using various tracer and nontracer modalities and can provide additional physiologic and hemodynamic information, which is not available with routine morphologic imaging. Tumor vascular perfusion parameters obtained by using CT or MR perfusion have been used for tumor grading, prognosis, and treatment response in addition to differentiating treatment/radiation effects and non-neoplastic lesions from neoplasms. This article is an overview of the utility of PCT for assessment of brain tumors and describes the technique, its advantages, and limitations.
Figures
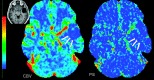
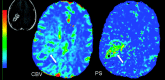
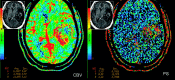
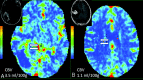
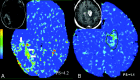

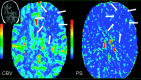
Similar articles
-
Dynamic perfusion CT in brain tumors.Eur J Radiol. 2015 Dec;84(12):2386-92. doi: 10.1016/j.ejrad.2015.02.012. Epub 2015 Feb 23. Eur J Radiol. 2015. PMID: 25796424 Review.
-
Comparison of the Effect of Vessel Size Imaging and Cerebral Blood Volume Derived from Perfusion MR Imaging on Glioma Grading.AJNR Am J Neuroradiol. 2016 Jan;37(1):51-7. doi: 10.3174/ajnr.A4477. Epub 2015 Sep 17. AJNR Am J Neuroradiol. 2016. PMID: 26381565 Free PMC article.
-
Diagnostic Accuracy of Perfusion Computed Tomography in Cerebral Glioma Grading.J Coll Physicians Surg Pak. 2016 Jul;26(7):562-5. J Coll Physicians Surg Pak. 2016. PMID: 27504544
-
Comparison of 18F-FET PET and perfusion-weighted MR imaging: a PET/MR imaging hybrid study in patients with brain tumors.J Nucl Med. 2014 Apr;55(4):540-5. doi: 10.2967/jnumed.113.129007. Epub 2014 Feb 27. J Nucl Med. 2014. PMID: 24578243
-
Clinical Review of Computed Tomography and MR Perfusion Imaging in Neuro-Oncology.Radiol Clin North Am. 2021 May;59(3):323-334. doi: 10.1016/j.rcl.2021.01.002. Epub 2021 Mar 23. Radiol Clin North Am. 2021. PMID: 33926680 Review.
Cited by
-
Current trends in the characterization and monitoring of vascular response to cancer therapy.Cancer Imaging. 2024 Oct 23;24(1):143. doi: 10.1186/s40644-024-00767-8. Cancer Imaging. 2024. PMID: 39438891 Free PMC article. Review.
-
The use of (18)F-FDG PET to differentiate progressive disease from treatment induced necrosis in high grade glioma.J Neurooncol. 2015 Oct;125(1):167-75. doi: 10.1007/s11060-015-1883-1. Epub 2015 Sep 18. J Neurooncol. 2015. PMID: 26384811 Free PMC article.
-
OS-DETR: End-to-end brain tumor detection framework based on orthogonal channel shuffle networks.PLoS One. 2025 May 13;20(5):e0320757. doi: 10.1371/journal.pone.0320757. eCollection 2025. PLoS One. 2025. PMID: 40359502 Free PMC article.
-
A stochastic model of blood flow to calculate blood dose during radiotherapy.Phys Med Biol. 2023 Nov 8;68(22):10.1088/1361-6560/ad02d6. doi: 10.1088/1361-6560/ad02d6. Phys Med Biol. 2023. PMID: 37827171 Free PMC article.
-
Pediatric posterior fossa incidentalomas.Childs Nerv Syst. 2020 Mar;36(3):601-609. doi: 10.1007/s00381-019-04364-0. Epub 2019 Sep 6. Childs Nerv Syst. 2020. PMID: 31492982
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
