Increased pericardial fat volume measured from noncontrast CT predicts myocardial ischemia by SPECT
- PMID: 21070997
- PMCID: PMC3057558
- DOI: 10.1016/j.jcmg.2010.07.014
Increased pericardial fat volume measured from noncontrast CT predicts myocardial ischemia by SPECT
Abstract
Objectives: We evaluated the association between pericardial fat and myocardial ischemia for risk stratification.
Background: Pericardial fat volume (PFV) and thoracic fat volume (TFV) measured from noncontrast computed tomography (CT) performed for calculating coronary calcium score (CCS) are associated with increased CCS and risk for major adverse cardiovascular events.
Methods: From a cohort of 1,777 consecutive patients without previously known coronary artery disease (CAD) with noncontrast CT performed within 6 months of single photon emission computed tomography (SPECT), we compared 73 patients with ischemia by SPECT (cases) with 146 patients with normal SPECT (controls) matched by age, gender, CCS category, and symptoms and risk factors for CAD. TFV was automatically measured. Pericardial contours were manually defined within which fat voxels were automatically identified to compute PFV. Computer-assisted visual interpretation of SPECT was performed using standard 17-segment and 5-point score model; perfusion defect was quantified as summed stress score (SSS) and summed rest score (SRS). Ischemia was defined by: SSS - SRS ≥4. Independent relationships of PFV and TFV to ischemia were examined.
Results: Cases had higher mean PFV (99.1 ± 42.9 cm(3) vs. 80.1 ± 31.8 cm(3), p = 0.0003) and TFV (196.1 ± 82.7 cm(3) vs. 160.8 ± 72.1 cm(3), p = 0.001) and higher frequencies of PFV >125 cm(3) (22% vs. 8%, p = 0.004) and TFV >200 cm(3) (40% vs. 19%, p = 0.001) than controls. After adjustment for CCS, PFV and TFV remained the strongest predictors of ischemia (odds ratio [OR]: 2.91, 95% confidence interval [CI]: 1.53 to 5.52, p = 0.001 for each doubling of PFV; OR: 2.64, 95% CI: 1.48 to 4.72, p = 0.001 for TFV). Receiver operating characteristic analysis showed that prediction of ischemia, as indicated by receiver-operator characteristic area under the curve, improved significantly when PFV or TFV was added to CCS (0.75 vs. 0.68, p = 0.04 for both).
Conclusions: Pericardial fat was significantly associated with myocardial ischemia in patients without known CAD and may help improve risk assessment.
Copyright © 2010 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Figures


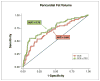
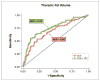
References
-
- Dey D, Suzuki Y, Suzuki S, et al. Automated quantitation of pericardiac fat from noncontrast CT. Invest Radiol. 2008;43:145–53. - PubMed
-
- Taguchi R, Takasu J, Itani Y, et al. Pericardial fat accumulation in men as a risk factor for coronary artery disease. Atherosclerosis. 2001;157:203–9. - PubMed
-
- Wheeler GL, Shi R, Beck SR, et al. Pericardial and visceral adipose tissues measured volumetrically with computed tomography are highly associated in type 2 diabetic families. Invest Radiol. 2005;40:97–101. - PubMed
-
- Fox CS, Massaro JM, Hoffmann U, et al. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation. 2007;116:39–48. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

