Decreased mortality resulting from a multicomponent intervention in a tertiary care medical intensive care unit
- PMID: 21076286
- PMCID: PMC3383659
- DOI: 10.1097/CCM.0b013e3181ffdd2f
Decreased mortality resulting from a multicomponent intervention in a tertiary care medical intensive care unit
Abstract
Objective: To evaluate whether a multicomponent intervention, particularly increasing staff, can achieve reductions in patient mortality in an already high-intensity, Leapfrog-compliant medical intensive care unit.
Design: Retrospective, observational study.
Setting: Medical intensive care unit of a tertiary care, academic medical center.
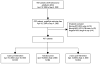
Patients: A total of 1,263 patients admitted between April 19, 2004 and April 18, 2006 (before the organizational change) were compared with 2,424 patients admitted between September 5, 2006 and September 4, 2008.
Interventions: A multicomponent intervention including the physical move from a 10-bed to a 29-bed medical intensive care unit with larger patient rooms, the initiation of 24-hr critical care specialist coverage in the medical intensive care unit, an increase in the respiratory therapist:patient ratio, and the addition of a clinical pharmacist to the multidisciplinary team.
Measurements and main results: Measurements were made based on mortality in the intensive care unit and in-hospital. Patient comorbidity as measured by the Charlson score did not change after the intervention (2.7 ± 2.7 vs. 2.8 ± 2.6, p = .62), nor did the acuity of illness as measured by the case mix index (3.0 ± 3.7 vs. 3.1 ± 3.8, p = .69). The unadjusted medical intensive care unit mortality decreased from 18.4% to 14.9% (p = .006), as did in-hospital mortality (from 25.8% to 21.7%, p = .005). The reduction in medical intensive care unit mortality was consistent in the multivariable regression with adjustment for multiple possible confounders (odds ratio = 0.74, 95% confidence interval: 0.61-0.91, p = .003), as was the reduction in hospital mortality (odds ratio = 0.74, 95% confidence interval: 0.62-0.88, p = .001). In mechanically ventilated patients, there was an increase in median 28-day ventilator-free days (21, interquartile range 0-25 vs. 22, interquartile range 0-26, p = .04). An increase in median medical intensive care unit (2.4, interquartile range 1.1-5.2 vs. 2.7, interquartile range 1.3-5.9), p = .009) but not hospital (8.3, interquartile range 4.1-17.0 vs. 8.2, interquartile range 4.0-16.8; p = .851) length of stay in days occurred with the intervention. The mean daily dosing of fentanyl and lorazepam decreased after the intervention.
Conclusions: A multicomponent reorganization of medical intensive care unit services was associated with important reductions in mortality for medical intensive care unit patients, as well as an increased number of ventilator-free days. Substantial and sustained changes in clinically important outcomes may be obtained from organizational changes.
Conflict of interest statement
The authors have not disclosed any potential conflicts of interest.
Figures
References
-
- Kahn JM, Goss CH, Heagerty PJ, et al. Hospital volume and the outcomes of mechanical ventilation. N Engl J Med. 2006;355:41–50. - PubMed
-
- Krumholz HM, Normand SL, Spertus JA, et al. Measuring performance for treating heart attacks and heart failure: The case for outcomes measurement. Health Affairs (Millwood) 2007;26:75–85. - PubMed
-
- McGrath PD, Wennberg DE, Dickens JD, Jr, et al. Relation between operator and hospital volume and outcomes following percutaneous coronary interventions in the era of the coronary stent. JAMA. 2000;284:3139–3144. - PubMed
-
- Magid DJ, Calonge BN, Rumsfeld JS, et al. Relation between hospital primary angioplasty volume and mortality for patients with acute MI treated with primary angioplasty vs thrombolytic therapy. JAMA. 2000;284:3131–3138. - PubMed
-
- Kumbhani DJ, Cannon CP, Fonarow GC, et al. Association of hospital primary angioplasty volume in ST-segment elevation myocardial infarction with quality and outcomes. JAMA. 2009;302:2207–2213. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous