Clinical outcome of cranial neuropathy in patients with pituitary apoplexy
- PMID: 21082047
- PMCID: PMC2966721
- DOI: 10.3340/jkns.2010.48.3.213
Clinical outcome of cranial neuropathy in patients with pituitary apoplexy
Abstract
Objective: Pituitary apoplexy (PA) is described as a clinical syndrome characterized by sudden headache, vomiting, visual impairment, and meningismus caused by rapid enlargement of a pituitary adenoma. We retrospectively analyzed the clinical presentation and surgical outcome in PA presenting with cranial neuropathy.
Methods: Twelve cases (3.3%) of PA were retrospectively reviewed among 359 patients diagnosed with pituitary adenoma. The study included 6 males and 6 females. Mean age of patients was 49.0 years, with a range of 16 to 74 years. Follow-up duration ranged from 3 to 20 months, with an average of 12 months. All patients were submitted to surgery, using the transsphenoidal approach (TSA).
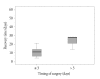
Results: Symptoms included abrupt headache (11/12), decreased visual acuity (12/12), visual field defect (11/12), and cranial nerve palsy of the third (5/12) and sixth (2/12). Mean height of the mass was 29.0 mm (range 15-46). Duration between the ictus and operation ranged from 1 to 15 days (mean 7.0). The symptom duration before operation and the recovery period of cranial neuropathy correlated significantly (p = 0.0286). TSA resulted in improvement of decreased visual acuity in 91.6%, visual field defect in 54.5%, and cranial neuropathy in 100% at 3 months after surgery.
Conclusion: PA is a rare event, complicating 3.3% in our series. Even in blindness following pituitary apoplexy cases, improvement of cranial neuropathy is possible if adequate management is initiated in time. Surgical decompression must be considered as soon as possible in cases with severe visual impairment or cranial neuropathy.
Keywords: Cranial neuropathy; Pituitary adenoma; Pituitary apoplexy; Transsphenoidal approach.
Figures

Similar articles
-
Classical pituitary apoplexy: clinical features, management and outcome.Clin Endocrinol (Oxf). 1999 Aug;51(2):181-8. doi: 10.1046/j.1365-2265.1999.00754.x. Clin Endocrinol (Oxf). 1999. PMID: 10468988
-
Recovery of Cranial Nerve Deficits in Patients Presenting with Pituitary Apoplexy: A Case Series.J Neurol Surg B Skull Base. 2021 Jan 21;83(Suppl 2):e1-e6. doi: 10.1055/s-0040-1722668. eCollection 2022 Jun. J Neurol Surg B Skull Base. 2021. PMID: 35832969 Free PMC article.
-
Management and outcomes of pituitary apoplexy.J Neurosurg. 2015 Jun;122(6):1450-7. doi: 10.3171/2014.10.JNS141204. Epub 2015 Apr 10. J Neurosurg. 2015. PMID: 25859804
-
Isolated Sixth Cranial Nerve Palsy in Patients with Pituitary Apoplexy.J Neurol Surg A Cent Eur Neurosurg. 2025 Jul;86(4):408-414. doi: 10.1055/s-0044-1791973. Epub 2024 Nov 8. J Neurol Surg A Cent Eur Neurosurg. 2025. PMID: 39515376 Review.
-
Pituitary Apoplexy: Results of Surgical and Conservative Management Clinical Series and Review of the Literature.World Neurosurg. 2019 Oct;130:e988-e999. doi: 10.1016/j.wneu.2019.07.055. Epub 2019 Jul 11. World Neurosurg. 2019. PMID: 31302273 Review.
Cited by
-
Pituitary apoplexy following mitral valvuloplasty.J Korean Neurosurg Soc. 2015 Apr;57(4):289-91. doi: 10.3340/jkns.2015.57.4.289. Epub 2015 Apr 24. J Korean Neurosurg Soc. 2015. PMID: 25932297 Free PMC article.
-
Pituitary apoplexy.Endocrine. 2015 Feb;48(1):69-75. doi: 10.1007/s12020-014-0359-y. Epub 2014 Jul 26. Endocrine. 2015. PMID: 25063308 Review.
-
Oculomotor outcomes of cranial nerve palsy in patients with skull base tumors.PLoS One. 2024 Aug 29;19(8):e0309686. doi: 10.1371/journal.pone.0309686. eCollection 2024. PLoS One. 2024. PMID: 39208348 Free PMC article.
-
Visual and Hormone Outcomes in Pituitary Apoplexy: Results of a Single Surgeon, Single Institution 15-Year Retrospective Review and Pooled Data Analysis.J Neurol Surg B Skull Base. 2020 Jun 19;82(4):392-400. doi: 10.1055/s-0040-1713104. eCollection 2021 Aug. J Neurol Surg B Skull Base. 2020. PMID: 35573926 Free PMC article.
-
A Case of Giant Pituitary Adenoma Associated with a Postoperative Mental Disorder That Ultimately Resulted in Bilateral Blindness.Case Rep Ophthalmol. 2020 Mar 4;11(1):92-99. doi: 10.1159/000506392. eCollection 2020 Jan-Apr. Case Rep Ophthalmol. 2020. PMID: 32308609 Free PMC article.
References
-
- Agrawal D, Mahapatra AK. Visual outcome of blind eyes in pituitary apoplexy after transsphenoidal surgery : a series of 14 eyes. Surg Neurol. 2005;63:42–46. discussion 46. - PubMed
-
- Arafah BM, Harrington JF, Madhoun ZT, Selman WR. Improvement of pituitary function after surgical decompression for pituitary tumor apoplexy. J Clin Endocrinol Metab. 1990;71:323–328. - PubMed
-
- Bills DC, Meyer FB, Laws ER, Jr, Davis DH, Ebersold MJ, Scheithauer BW, et al. A retrospective analysis of pituitary apoplexy. Neurosurgery. 1993;33:602–608. discussion 608-609. - PubMed
-
- Brisman MH, Katz G, Post KD. Symptoms of pituitary apoplexy rapidly reversed with bromocriptine. case report. J Neurosurg. 1996;85:1153–1155. - PubMed
-
- Cardoso ER, Peterson EW. Pituitary apoplexy : a review. Neurosurgery. 1984;14:363–373. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

