Fluoroscopic management of complications after colorectal stent placement
- PMID: 21103302
- PMCID: PMC2989549
- DOI: 10.5009/gnl.2010.4.S1.S9
Fluoroscopic management of complications after colorectal stent placement
Abstract
Colorectal self-expanding metal stents have been widely used as a bridge to surgery in patients with acute malignant colonic obstruction by allowing a single-stage operation, or as a definitive palliative procedure in patients with inoperable tumors. Colonic stents are placed under either fluoroscopic or combined endoscopic and fluoroscopic guidance, with similar technical-success and complication rates. Placement of colonic stents is a very safe procedure with a low procedure-related mortality rate, but serious complications can develop and reinterventions are not uncommon. Most of the complications can be treated by minimally invasive or conservative techniques, while surgical interventions are required for most patients with perforation.
Keywords: Colorectal cancer; Complications; Self-expandable metal stents.
Figures
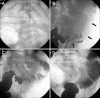
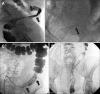
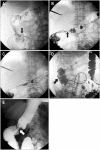

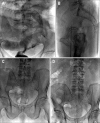
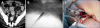
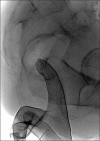
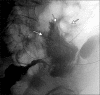

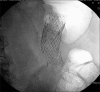

Similar articles
-
Outcomes and complications of self-expanding metal stent placement for malignant colonic obstruction in a single-center study.Wideochir Inne Tech Maloinwazyjne. 2018 Mar;13(1):53-56. doi: 10.5114/wiitm.2017.70194. Epub 2017 Sep 26. Wideochir Inne Tech Maloinwazyjne. 2018. PMID: 29643958 Free PMC article.
-
Short- and long-term clinical outcomes of self-expandable metal stents inserted for colorectal obstruction and efficacy of different insertion techniques.Gastroenterol Hepatol. 2019 Mar;42(3):157-163. doi: 10.1016/j.gastrohep.2018.07.014. Epub 2018 Oct 9. Gastroenterol Hepatol. 2019. PMID: 30314765 English, Spanish.
-
Endoscopic placement of self-expandable metal stents for malignant colonic obstruction: long-term outcomes and complication factors.Gastrointest Endosc. 2010 Mar;71(3):560-72. doi: 10.1016/j.gie.2009.10.012. Gastrointest Endosc. 2010. PMID: 20189515
-
Role of self expandable stents in management of colorectal cancers.World J Gastrointest Oncol. 2016 Jan 15;8(1):113-20. doi: 10.4251/wjgo.v8.i1.113. World J Gastrointest Oncol. 2016. PMID: 26798442 Free PMC article. Review.
-
Update on the indications and use of colonic stents.Curr Gastroenterol Rep. 2010 Oct;12(5):374-82. doi: 10.1007/s11894-010-0136-x. Curr Gastroenterol Rep. 2010. PMID: 20703837 Review.
Cited by
-
Clinical impact of prophylactic antibiotic treatment for self-expandable metallic stent insertion in patients with malignant colorectal obstruction.Gastroenterol Res Pract. 2015;2015:416142. doi: 10.1155/2015/416142. Epub 2015 Mar 31. Gastroenterol Res Pract. 2015. PMID: 25918522 Free PMC article.
-
Angular positioning of stent increases bowel perforation after self-expandable metal stent placement for malignant colorectal obstruction.Clin Endosc. 2013 Jul;46(4):384-9. doi: 10.5946/ce.2013.46.4.384. Epub 2013 Jul 31. Clin Endosc. 2013. PMID: 23964336 Free PMC article.
-
Clinical outcomes following secondary self-expandable metal stent (SEMS) insertion due to previous stent migration in malignant colorectal obstruction.Surg Endosc. 2013 Sep;27(9):3288-96. doi: 10.1007/s00464-013-2907-6. Epub 2013 Mar 22. Surg Endosc. 2013. PMID: 23519493
-
Evidence-based recommendations on colorectal stenting: a report from the stent study group of the korean society of gastrointestinal endoscopy.Clin Endosc. 2013 Jul;46(4):355-67. doi: 10.5946/ce.2013.46.4.355. Epub 2013 Jul 31. Clin Endosc. 2013. PMID: 23964332 Free PMC article.
-
Newly designed flared-end covered versus uncovered self-expandable metallic stents for palliation of malignant colorectal obstruction: a randomized, prospective study.Intest Res. 2025 Apr;23(2):202-212. doi: 10.5217/ir.2024.00135. Epub 2025 Feb 24. Intest Res. 2025. PMID: 39988445 Free PMC article.
References
-
- Sebastian S, Johnston S, Geoghegan T, Torreggiani W, Buckley M. Pooled analysis of the efficacy and safety of self-expanding metal stenting in malignant colorectal obstruction. Am J Gastroenterol. 2004;99:2051–2057. - PubMed
-
- Kim H, Kim SH, Choi SY, et al. Fluoroscopically guided placement of self-expandable metallic stents and stent-grafts in the treatment of acute malignant colorectal obstruction. J Vasc Interv Radiol. 2008;19:1709–1716. - PubMed
-
- Baron TH. Interventional palliative strategies for malignant bowel obstruction. Curr Oncol Rep. 2009;11:293–297. - PubMed
-
- Small AJ, Coelho-Prabhu N, Baron TH. Endoscopic placement of self-expandable metal stents for malignant colonic obstruction: long-term outcomes and complication factors. Gastrointest Endosc. 2010;71:560–572. - PubMed
-
- Small AJ, Baron TH. Comparison of Wallstent and Ultraflex stents for palliation of malignant left-sided colon obstruction: a retrospective, case-matched analysis. Gastrointest Endosc. 2008;67:478–488. - PubMed
LinkOut - more resources
Full Text Sources

