Integrating tobacco cessation into mental health care for posttraumatic stress disorder: a randomized controlled trial
- PMID: 21139110
- PMCID: PMC4218733
- DOI: 10.1001/jama.2010.1769
Integrating tobacco cessation into mental health care for posttraumatic stress disorder: a randomized controlled trial
Abstract
Context: Most smokers with mental illness do not receive tobacco cessation treatment.
Objective: To determine whether integrating smoking cessation treatment into mental health care for veterans with posttraumatic stress disorder (PTSD) improves long-term smoking abstinence rates.
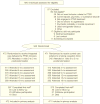
Design, setting, and patients: A randomized controlled trial of 943 smokers with military-related PTSD who were recruited from outpatient PTSD clinics at 10 Veterans Affairs medical centers and followed up for 18 to 48 months between November 2004 and July 2009.
Intervention: Smoking cessation treatment integrated within mental health care for PTSD delivered by mental health clinicians (integrated care [IC]) vs referral to Veterans Affairs smoking cessation clinics (SCC). Patients received smoking cessation treatment within 3 months of study enrollment.
Main outcome measures: Smoking outcomes included 12-month bioverified prolonged abstinence (primary outcome) and 7- and 30-day point prevalence abstinence assessed at 3-month intervals. Amount of smoking cessation medications and counseling sessions delivered were tested as mediators of outcome. Posttraumatic stress disorder and depression were repeatedly assessed using the PTSD Checklist and Patient Health Questionnaire 9, respectively, to determine if IC participation or quitting smoking worsened psychiatric status.
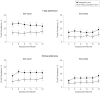
Results: Integrated care was better than SCC on prolonged abstinence (8.9% vs 4.5%; adjusted odds ratio, 2.26; 95% confidence interval [CI], 1.30-3.91; P = .004). Differences between IC vs SCC were largest at 6 months for 7-day point prevalence abstinence (78/472 [16.5%] vs 34/471 [7.2%], P < .001) and remained significant at 18 months (86/472 [18.2%] vs 51/471 [10.8%], P < .001). Number of counseling sessions received and days of cessation medication used explained 39.1% of the treatment effect. Between baseline and 18 months, psychiatric status did not differ between treatment conditions. Posttraumatic stress disorder symptoms for quitters and nonquitters improved. Nonquitters worsened slightly on the Patient Health Questionnaire 9 relative to quitters (differences ranged between 0.4 and 2.1, P = .03), whose scores did not change over time.
Conclusion: Among smokers with military-related PTSD, integrating smoking cessation treatment into mental health care compared with referral to specialized cessation treatment resulted in greater prolonged abstinence.
Trial registration: clinicaltrials.gov Identifier: NCT00118534.
Figures

Comment in
-
Integrating tobacco treatment into mental health settings.JAMA. 2010 Dec 8;304(22):2534-5. doi: 10.1001/jama.2010.1759. JAMA. 2010. PMID: 21139117 Free PMC article. No abstract available.
References
-
- Ziedonis D, Hitsman B, Beckham JC, et al. Tobacco use and cessation in psychiatric disorders. Nicotine Tob Res. 2008;10(12):1691–1715. - PubMed
-
- Kessler RC, Berglund P, Demler O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):593–602. - PubMed
-
- Lasser K, Boyd JW, Woolhandler S, et al. Smoking and mental illness: a population-based prevalence study. JAMA. 2000;284(20):2606–2610. - PubMed
-
- Beckham JC, Kirby AC, Feldman ME, et al. Prevalence and correlates of heavy smoking in Vietnam veterans with chronic posttraumatic stress disorder. Addict Behav. 1997;22(5):637–647. - PubMed
-
- Feldner MT, Babson KA, Zvolensky MJ, et al. Post-traumatic stress symptoms and smoking to reduce negative affect. Addict Behav. 2007;32(2):214–227. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

