Imaging considerations in intraductal papillary mucinous neoplasms of the pancreas
- PMID: 21160838
- PMCID: PMC2999202
- DOI: 10.4240/wjgs.v2.i10.324
Imaging considerations in intraductal papillary mucinous neoplasms of the pancreas
Abstract
With the widespread use of cross-sectional imaging, particularly computed tomography (CT) and magnetic resonance imaging (MRI), and the continuous improvement in the image quality of these techniques, the diagnosis of incidental pancreatic cysts has increased dramatically in the last decades. While the vast majority of these cysts are not clinically relevant, a small percentage of them will evolve into an invasive malignant tumor making their management challenging. Mucinous cystic neoplasms and intraductal papillary mucinous neoplasms (IPMN) are the most common pancreatic cystic lesions with malignant potential. Imaging findings on CT and MRI correlate tightly with the presence of malignant degeneration in these neoplasms. IPMN can be classified based on their distribution as main duct, branch duct or mixed type lesions. MRI is superior to CT in demonstrating the communication of a branch duct IPMN with the main pancreatic duct (MPD). Most branch duct lesions are benign whereas tumors involving the MPD are frequently associated with malignancy. The presence of solid nodules, thick enhancing walls and/or septae, a wide (> 1 cm) connection of a side-branch lesion with the MPD and the size of the tumor > 3 cm are indicative of malignancy in a branch and mixed type IPMN. A main pancreatic duct > 6 mm, a mural nodule > 3 mm and an abnormal attenuating area in the adjacent pancreatic parenchyma on CT correlates with malignant disease in main duct and mixed type IPMN. An accurate characterization of these neoplasms by imaging is thus crucial for selecting the best management options. In this article, we review the imaging findings of IPMN including imaging predictors of malignancy and surgical resectability. We also discuss follow-up strategies for patients with surgically resected IPMN and patients with incidental pancreatic cysts.
Keywords: Computed tomography; Intraductal papillary mucinous neoplasms; Magnetic resonance imaging; Pancreatic neoplasms.
Figures

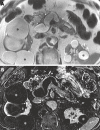
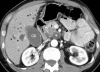
References
-
- Lee KS, Sekhar A, Rofsky NM, Pedrosa I. Prevalence of incidental pancreatic cysts in the adult population on MR imaging. Am J Gastroenterol. 2010;105:2079–2084. - PubMed
-
- Zhang XM, Mitchell DG, Dohke M, Holland GA, Parker L. Pancreatic cysts: depiction on single-shot fast spin-echo MR images. Radiology. 2002;223:547–553. - PubMed
-
- Handrich SJ, Hough DM, Fletcher JG, Sarr MG. The natural history of the incidentally discovered small simple pancreatic cyst: long-term follow-up and clinical implications. AJR Am J Roentgenol. 2005;184:20–23. - PubMed
-
- Tanno S, Nakano Y, Nishikawa T, Nakamura K, Sasajima J, Minoguchi M, Mizukami Y, Yanagawa N, Fujii T, Obara T, et al. Natural history of branch duct intraductal papillary-mucinous neoplasms of the pancreas without mural nodules: long-term follow-up results. Gut. 2008;57:339–343. - PubMed
LinkOut - more resources
Full Text Sources

