VEGFR2 and Src kinase inhibitors suppress Andes virus-induced endothelial cell permeability
- PMID: 21177802
- PMCID: PMC3067787
- DOI: 10.1128/JVI.02319-10
VEGFR2 and Src kinase inhibitors suppress Andes virus-induced endothelial cell permeability
Abstract
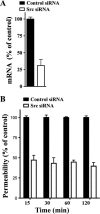
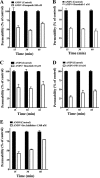
Hantaviruses predominantly infect human endothelial cells and, in the absence of cell lysis, cause two diseases resulting from increased vascular permeability. Andes virus (ANDV) causes a highly lethal acute pulmonary edema termed hantavirus pulmonary syndrome (HPS). ANDV infection enhances the permeability of endothelial cells in response to vascular endothelial growth factor (VEGF) by increasing signaling responses directed by the VEGFR2-Src-VE-cadherin pathway, which directs adherens junction (AJ) disassembly. Here we demonstrate that inhibiting pathway-specific VEGFR2 and Src family kinases (SFKs) blocks ANDV-induced endothelial cell permeability. Small interfering RNA (siRNA) knockdown of Src within ANDV-infected endothelial cells resulted in an ∼70% decrease in endothelial cell permeability compared to that for siRNA controls. This finding suggested that existing FDA-approved small-molecule kinase inhibitors might similarly block ANDV-induced permeability. The VEGFR2 kinase inhibitor pazopanib as well as SFK inhibitors dasatinib, PP1, bosutinib, and Src inhibitor 1 dramatically inhibited ANDV-induced endothelial cell permeability. Consistent with their kinase-inhibitory concentrations, dasatinib, PP1, and pazopanib inhibited ANDV-induced permeability at 1, 10, and 100 nanomolar 50% inhibitory concentrations (IC(50)s), respectively. We further demonstrated that dasatinib and pazopanib blocked VE-cadherin dissociation from the AJs of ANDV-infected endothelial cells by >90%. These findings indicate that VEGFR2 and Src kinases are potential targets for therapeutically reducing ANDV-induced endothelial cell permeability and, as a result, capillary permeability during HPS. Since the functions of VEGFR2 and SFK inhibitors are already well defined and FDA approved for clinical use, these findings rationalize their therapeutic evaluation for efficacy in reducing HPS disease. Endothelial cell barrier functions are disrupted by a number of viruses that cause hemorrhagic, edematous, or neurologic disease, and as a result, our findings suggest that VEGFR2 and SFK inhibitors should be considered for regulating endothelial cell barrier functions altered by additional viral pathogens.
Figures


References
-
- Adjei, A. A. 2007. Novel small-molecule inhibitors of the vascular endothelial growth factor receptor. Clin. Lung Cancer 8(Suppl. 2):S74-S78. - PubMed
-
- Berger, M. M., et al. 2005. Hypoxia impairs systemic endothelial function in individuals prone to high-altitude pulmonary edema. Am. J. Respir. Crit. Care Med. 172:763-767. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

