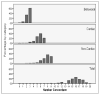
Patient perception versus medical record entry of health-related conditions among patients with heart failure
- PMID: 21185003
- PMCID: PMC3683070
- DOI: 10.1016/j.amjcard.2010.10.017
Patient perception versus medical record entry of health-related conditions among patients with heart failure
Abstract
A shared understanding of medical conditions between patients and their health care providers may improve self-care and outcomes. In this study, the concordance between responses to a medical history self-report (MHSR) form and the corresponding provider documentation in electronic health records (EHRs) of 19 select co-morbidities and habits in 230 patients with heart failure were evaluated. Overall concordance was assessed using the κ statistic, and crude, positive, and negative agreement were determined for each condition. Concordance between MHSR and EHR varied widely for cardiovascular conditions (κ = 0.37 to 0.96), noncardiovascular conditions (κ = 0.06 to 1.00), and habits (κ = 0.26 to 0.69). Less than 80% crude agreement was seen for history of arrhythmias (72%), dyslipidemia (74%), and hypertension (79%) among cardiovascular conditions and lung disease (70%) and peripheral arterial disease (78%) for noncardiovascular conditions. Perfect agreement was observed for only 1 of the 19 conditions (human immunodeficiency virus status). Negative agreement >80% was more frequent than >80% positive agreement for a condition (15 of 19 [79%] vs 8 of 19 [42%], respectively, p = 0.02). Only 20% of patients had concordant MSHRs and EHRs for all 7 cardiovascular conditions; in 40% of patients, concordance was observed for ≤5 conditions. For noncardiovascular conditions, only 28% of MSHR-EHR pairs agreed for all 9 conditions; 37% agreed for ≤7 conditions. Cumulatively, 39% of the pairs matched for ≤15 of 19 conditions. In conclusion, there is significant variation in the perceptions of patients with heart failure compared to providers' records of co-morbidities and habits. The root causes of this variation and its impact on outcomes need further study.
Copyright © 2011 Elsevier Inc. All rights reserved.
Figures
References
-
- Lloyd-Jones D, Adams R, Brown T, Carnethon M, Dai S, De Simone G, Ferguson T, Ford E, Furie K, Gillespie C, Go A, Greenlund K, Haase N, Hailpern S, Ho P, Howard V, Kissela B, Kittner S, Lackland D, Lisabeth L, Marelli A, McDermott M, Meigs J, Mozaffarian D, Mussolino M, Nichol G, Roger V, Rosamond W, Sacco R, Sorlie P, Stafford R, Thom T, Wasserthiel-Smoller S, Wong N, Wylie-Rosett J. Heart disease and stroke statistics—2010 update: a report from the American Heart Association. Circulation. 2010;121:e46– e215. - PubMed
-
- Liu L. Changes in cardiovascular hospitalization and comorbidity of heart failure in the United States: findings from the National Hospital Discharge Surveys 1980–2006. Int J Cardiol. In press. - PubMed
-
- Epstein R, Alper B, Quill T. Communicating evidence for participatory decision making. JAMA. 2004;291:2359–2366. - PubMed
-
- Baker D, Asch S, Keesey J, Brown J, Chan K, Joyce G, Keeler E. Differences in education, knowledge, self-management activities, and health outcomes for patients with heart failure cared for under the chronic disease model: the improving chronic illness care evaluation. J Card Fail. 2005;11:405–413. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical