Rates of initial virological suppression and subsequent virological failure after initiating highly active antiretroviral therapy: the impact of aboriginal ethnicity and injection drug use
- PMID: 21187007
- PMCID: PMC4428381
- DOI: 10.2174/157016210794088227
Rates of initial virological suppression and subsequent virological failure after initiating highly active antiretroviral therapy: the impact of aboriginal ethnicity and injection drug use
Abstract
Objectives: To compare rates of initial virological suppression and subsequent virological failure by Aboriginal ethnicity after starting highly active antiretroviral therapy (HAART).
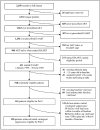
Methods: We conducted a retrospective cohort study of antiretroviral-naïve HIV-patients starting HAART in January 1999-June 2005 (baseline), followed until December 31, 2005 in Alberta, Canada. We compared the odds of achieving initial virological suppression (viral load <500 copies/mL) by Aboriginal ethnicity using logistic regression and, among those achieving suppression, rates of virological failure (the first of two consecutive viral loads >1000 copies/mL) by Aboriginal ethnicity using cumulative incidence curves and Cox proportional hazards models. Sex, injection drug use as an HIV exposure category (IDU), baseline age, CD4 cell count, viral load, calendar year, and HAART regimen were considered as potential confounders.
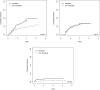
Results: Of 461 study patients, 37% were Aboriginal and 48% were IDUs; 71% achieved initial virological suppression and were followed for 730.4 person-years. After adjusting for confounding variables, compared to non-Aboriginals with other exposures, the odds of achieving initial virological suppression were lower for Aboriginal IDUs (odds ratio (OR)=0.33, 95% CI=0.19-0.60, p=0.0002), non-Aboriginal IDUs (OR=0.30, 95% CI=0.15-0.60, p=0.0006), and Aboriginals with other exposures (OR=0.38, 95% CI=0.21-0.67, p=0.0009). Among those achieving suppression, Aboriginals experienced higher virological failure rates ≥1 year after suppression (hazard ratio=3.35, 95% CI=1.68-6.65, p=0.0006).
Conclusions: Future research should investigate adherence among Aboriginals and IDUs treated with HAART and explore their treatment experiences to assess ways to improve outcomes.
Figures
References
-
- Martin L.J., Houston S., Yasui Y., Wild T.C., Saunders L.D. All-cause and HIV-related mortality rates among HIV-infected patients after initiating highly active antiretroviral therapy: the impact of Aboriginal ethnicity and injection drug use. Can. J. Public Health. 2011;102(2):90–96. - PMC - PubMed
-
- Lima V.D., Kretz P., Palepu A., Bonner S., Kerr T., Moore D., Daniel M., Montaner J.S., Hogg R.S., et al. Aboriginal status is a prognostic factor for mortality among antiretroviral naïve HIV-positive individuals first initiating HAART. AIDS Res. Ther. 2006;3:14. doi: 10.1186/1742-6405-3-14. - DOI - PMC - PubMed
-
- Panel on Antiretroviral Guidelines for Adults and Adolescents.Guidelines for the Use of Antiretroviral Agents in HIV-Infected Adults and Adolescents Available from: http://aidsinfo.nih.gov/contentfiles/AdultandAd olescentGL.pdf . [November 3, 2008 [cited 12 Mar 2009]].
-
- Public Health Agency of Canada; 2007. Public Health Agency of Canada, HIV/AIDS Epi Updates, November 2007. Surveillance and Risk Assessment Division, Centre for Infectious Disease Prevention and Control,
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials