Factors associated with trauma center use for elderly patients with trauma: a statewide analysis, 1999-2008
- PMID: 21242421
- PMCID: PMC3121677
- DOI: 10.1001/archsurg.2010.311
Factors associated with trauma center use for elderly patients with trauma: a statewide analysis, 1999-2008
Abstract
Objectives: To estimate the likelihood of trauma center admission for injured elderly patients with trauma, determine trends in trauma center admissions, and identify factors associated with trauma center use for elderly patients with trauma.
Design: Retrospective analysis.
Setting: Acute care hospitals in California.
Patients: All patients hospitalized for acute traumatic injuries during the period from January 1, 1999, to December 31, 2008 (n = 430,081). Patients who had scheduled admissions for nonacute or minor trauma were excluded.
Main outcome measure: Likelihood of admission to level I or II trauma center was calculated according to age categories after adjusting for patient and system factors.
Results: Of 430,081 patients admitted to California acute care hospitals for trauma-related diagnoses, 27% were older than 65 years. After adjusting for demographic, clinical, and system factors, compared with trauma patients aged 18-25 years, the odds of admission to a trauma center decreased with increasing age; patients aged 26-45 years had lower odds (odds ratio [OR], 0.75; 95% confidence interval [CI], 0.71-0.80) of being admitted to a trauma center for their injuries than did patients 46-65 years of age (OR, 0.57; 95% CI, 0.54-0.60), patients 66-85 years of age (OR, 0.35; 95% CI, 0.30-0.41), and patients older than 85 years (OR, 0.30; 95% CI, 0.25-0.36). Similar patterns were found when stratifying the analysis by trauma type and severity. Living more than 50 miles away from a trauma center (OR, 0.03; 95% CI, 0.01-0.06) and lack of county trauma center (OR, 0.17; 95% CI, 0.09-0.35) were also predictors of not receiving trauma care.
Conclusion: Age and likelihood of admission to a trauma center for injured patients were observed to be inversely proportional after controlling for other factors. System-level factors play a major role in determining which injured patients receive trauma care.
Figures
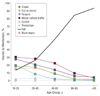



Comment in
-
Mortality in the elderly.Arch Surg. 2011 May;146(5):592-3. doi: 10.1001/archsurg.2011.70. Arch Surg. 2011. PMID: 21739656 No abstract available.
Similar articles
-
Mortality in the elderly.Arch Surg. 2011 May;146(5):592-3. doi: 10.1001/archsurg.2011.70. Arch Surg. 2011. PMID: 21739656 No abstract available.
-
Disparities in trauma center access despite increasing utilization: data from California, 1999 to 2006.J Trauma. 2010 Jan;68(1):217-24. doi: 10.1097/TA.0b013e3181a0e66d. J Trauma. 2010. PMID: 19901854 Free PMC article.
-
The Epidemiology of Emergency Department Trauma Discharges in the United States.Acad Emerg Med. 2017 Oct;24(10):1244-1256. doi: 10.1111/acem.13223. Epub 2017 Sep 27. Acad Emerg Med. 2017. PMID: 28493608 Free PMC article.
-
Factors associated with the disposition of severely injured patients initially seen at non–trauma center emergency departments: disparities by insurance status.JAMA Surg. 2014 May;149(5):422-30. doi: 10.1001/jamasurg.2013.4398. JAMA Surg. 2014. PMID: 24554059 Free PMC article.
-
Variability in pediatric utilization of trauma facilities in California: 1999 to 2005.Ann Emerg Med. 2008 Dec;52(6):607-15. doi: 10.1016/j.annemergmed.2008.05.011. Epub 2008 Jun 18. Ann Emerg Med. 2008. PMID: 18562043
Cited by
-
Association between trail use and self-rated wellness and health.BMC Public Health. 2020 Jan 30;20(1):128. doi: 10.1186/s12889-020-8273-0. BMC Public Health. 2020. PMID: 32000732 Free PMC article.
-
Impact of delayed mobile medical team dispatch for respiratory distress calls: a propensity score matched study from a French emergency communication center.Scand J Trauma Resusc Emerg Med. 2024 Apr 12;32(1):27. doi: 10.1186/s13049-024-01201-5. Scand J Trauma Resusc Emerg Med. 2024. PMID: 38609957 Free PMC article.
-
Factors Associated With Nontransfer in Trauma Patients Meeting American College of Surgeons' Criteria for Transfer at Nontertiary Centers.JAMA Surg. 2017 Apr 1;152(4):369-376. doi: 10.1001/jamasurg.2016.4976. JAMA Surg. 2017. PMID: 28052158 Free PMC article.
-
Helicopter emergency medical service dispatch in older trauma: time to reconsider the trigger?Scand J Trauma Resusc Emerg Med. 2021 May 7;29(1):62. doi: 10.1186/s13049-021-00877-3. Scand J Trauma Resusc Emerg Med. 2021. PMID: 33962682 Free PMC article.
-
Ten-year trends in traumatic brain injury: a retrospective cohort study of California emergency department and hospital revisits and readmissions.BMJ Open. 2018 Dec 14;8(12):e022297. doi: 10.1136/bmjopen-2018-022297. BMJ Open. 2018. PMID: 30552250 Free PMC article.
References
-
- McGwin G, Jr, Melton SM, May AK, Rue LW. Long-term survival in the elderly after trauma. J Trauma. 2000;49(3):470–476. - PubMed
-
- Hannan EL, Waller CH, Farrell LS, Rosati C. Elderly trauma inpatients in New York state: 1994–1998. J Trauma. 2004;56(6):1297–1304. - PubMed
-
- Mann NC, Cahn RM, Mullins RJ, Brand DM, Jurkovich GJ. Survival among injured geriatric patients during construction of a statewide trauma system. J Trauma. 2001;50(6):1111–1116. - PubMed
-
- DiRusso S, Holly C, Kamath R, et al. Preparation and achievement of American College of Surgeons level I trauma verification raises hospital performance and improves patient outcome. J Trauma. 2001;51(2):294–300. - PubMed
-
- Meldon SW, Reilly M, Drew BL, Mancuso C, Fallon W., Jr Trauma in the very elderly: a community-based study of outcomes at trauma and nontrauma centers. J Trauma. 2002;52(1):79–84. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

