Ventricular tachyarrhythmias after cardiac arrest in public versus at home
- PMID: 21268723
- PMCID: PMC3062845
- DOI: 10.1056/NEJMoa1010663
Ventricular tachyarrhythmias after cardiac arrest in public versus at home
Abstract
Background: The incidence of ventricular fibrillation or pulseless ventricular tachycardia as the first recorded rhythm after out-of-hospital cardiac arrest has unexpectedly declined. The success of bystander-deployed automated external defibrillators (AEDs) in public settings suggests that this may be the more common initial rhythm when out-of-hospital cardiac arrest occurs in public. We conducted a study to determine whether the location of the arrest, the type of arrhythmia, and the probability of survival are associated.
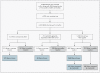
Methods: Between 2005 and 2007, we conducted a prospective cohort study of out-of-hospital cardiac arrest in adults in 10 North American communities. We assessed the frequencies of ventricular fibrillation or pulseless ventricular tachycardia and of survival to hospital discharge for arrests at home as compared with arrests in public.
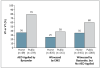
Results: Of 12,930 evaluated out-of-hospital cardiac arrests, 2042 occurred in public and 9564 at home. For cardiac arrests at home, the incidence of ventricular fibrillation or pulseless ventricular tachycardia was 25% when the arrest was witnessed by emergency-medical-services (EMS) personnel, 35% when it was witnessed by a bystander, and 36% when a bystander applied an AED. For cardiac arrests in public, the corresponding rates were 38%, 60%, and 79%. The adjusted odds ratio for initial ventricular fibrillation or pulseless ventricular tachycardia in public versus at home was 2.28 (95% confidence interval [CI], 1.96 to 2.66; P < 0.001) for bystander-witnessed arrests and 4.48 (95% CI, 2.23 to 8.97; P<0.001) for arrests in which bystanders applied AEDs. The rate of survival to hospital discharge was 34% for arrests in public settings with AEDs applied by bystanders versus 12% for arrests at home (adjusted odds ratio, 2.49; 95% CI, 1.03 to 5.99; P = 0.04).
Conclusions: Regardless of whether out-of-hospital cardiac arrests are witnessed by EMS personnel or bystanders and whether AEDs are applied by bystanders, the proportion of arrests with initial ventricular fibrillation or pulseless ventricular tachycardia is much greater in public settings than at home. The incremental value of resuscitation strategies, such as the ready availability of an AED, may be related to the place where the arrest occurs.
Figures
Comment in
-
A critic's assessment of our approach to cardiac arrest.N Engl J Med. 2011 Jan 27;364(4):374-5. doi: 10.1056/NEJMe1012554. N Engl J Med. 2011. PMID: 21268731 No abstract available.
-
Arrhythmias: home AEDs-a question of rhythm?Nat Rev Cardiol. 2011 Mar;8(3):124. doi: 10.1038/nrcardio.2011.18. Nat Rev Cardiol. 2011. PMID: 21475325 No abstract available.
-
Cardiac arrest in public versus at home.N Engl J Med. 2011 Apr 28;364(17):1674; author reply 1675-6. doi: 10.1056/NEJMc1102188. N Engl J Med. 2011. PMID: 21524220 No abstract available.
References
-
- Cobb LA, Fahrenbruch CE, Olsufka M, Copass MK. Changing incidence of out-of-hospital ventricular fibrillation, 1980-2000. JAMA. 2002;288:3008–13. - PubMed
-
- Becker L, Gold LS, Eisenberg M, White L, Hearne T, Rea T. Ventricular fibrillation in King County, Washington: a 30-year perspective. Resuscitation. 2008;79:22–7. - PubMed
-
- Heart and stroke statistics — 2010 update: a report from the American Heart Association. Circulation. 2010;121(7):e46–e215. - PubMed
Publication types
MeSH terms
Grants and funding
- U01 HL077866/HL/NHLBI NIH HHS/United States
- U01 HL077871/HL/NHLBI NIH HHS/United States
- HL077867/HL/NHLBI NIH HHS/United States
- 5U01 HL077863/HL/NHLBI NIH HHS/United States
- HL077887/HL/NHLBI NIH HHS/United States
- U01 HL077881/HL/NHLBI NIH HHS/United States
- HL077873/HL/NHLBI NIH HHS/United States
- HL077871/HL/NHLBI NIH HHS/United States
- HL077881/HL/NHLBI NIH HHS/United States
- HL077908/HL/NHLBI NIH HHS/United States
- U01 HL077887/HL/NHLBI NIH HHS/United States
- U01 HL077885/HL/NHLBI NIH HHS/United States
- CAPMC/ CIHR/Canada
- U01 HL077865/HL/NHLBI NIH HHS/United States
- U01 HL077863/HL/NHLBI NIH HHS/United States
- U01 HL077908/HL/NHLBI NIH HHS/United States
- HL077872/HL/NHLBI NIH HHS/United States
- HL077866/HL/NHLBI NIH HHS/United States
- U01 HL077873/HL/NHLBI NIH HHS/United States
- U01 HL077867/HL/NHLBI NIH HHS/United States
- HL077885/HL/NHLBI NIH HHS/United States
- HL077865/HL/NHLBI NIH HHS/United States
- U01 HL077872/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
