Role of 'Spot Sign' on CT Angiography to Predict Hematoma Expansion in Spontaneous Intracerebral Hemorrhage
- PMID: 21286475
- PMCID: PMC3030078
- DOI: 10.3340/jkns.2010.48.5.399
Role of 'Spot Sign' on CT Angiography to Predict Hematoma Expansion in Spontaneous Intracerebral Hemorrhage
Abstract
Objective: Patients with spontaneous intracerebral hemorrhage (ICH) presenting within 24 hours of symptom onset are known to be increased risk of hematoma expansion which is closely correlated with morbidity and mortality. We investigated whether tiny enhancing foci ('Spot sign') on axial view of 3-dimensional computed tomography angiography (3D-CTA) source images can predict subsequent hematoma expansion in spontaneous ICH.
Methods: During a 2-year period (March 2007-March 2009), we prospectively evaluated 3D-CTA of 110 patients with spontaneous ICH. Based on source images of 3D-CTA, patients were classified according to presence or absence of 'Spot sign'; 'Spot sign' (+) group, 'Spot sign' (-) group. Radiological factors and clinical outcomes were compared between two groups.
Results: Hematoma expansion occurred in 16 patients (15%). Mean Glasgow Coma Scale (GCS) score of patients with hematoma expansion was significantly different compared to score of patients without hematoma expansion (5 vs. 9, p < 0.001). Nineteen patients (16%) of 110 ICH patients demonstrated 'spot sign' on 3D-CTA. Among the 'spot sign' (+) group, 53% of patients developed hematoma expansion. Conversely 7% of patients without 'spot sign' demonstrated the hematoma expansion (p < 0.001). Initial volume and location of hematoma were significantly not associated with hematoma expansion except shape of hematoma.
Conclusion: Our study showed that patients with hematoma expansion of spontaneous ICH had significant clinical deterioration. And the fact that 'spot sign' (+) group have higher risk of hematoma expansion suggests the presence of 'spot sign' on source images of 3D-CTA can give a clue to predict hematoma expansion in spontaneous ICH.
Keywords: Computed tomography angiography; Hematoma expansion; Intracerebral hemorrhage; Prognosis.
Figures
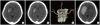

References
-
- Bae HG, Lee KS, Yun IG, Bae WK, Choi SK, Byun BJ, et al. Rapid expansion of hypertensive intracerebral hemorrhage. Neurosurgery. 1992;31:35–41. - PubMed
-
- Becker KJ, Baxter AB, Bybee HM, Tirschwell DL, Abouelsaad T, Cohen WA. Extravasation of radiographic contrast is an independent predictor of death in primary intracerebral hemorrhage. Stroke. 1999;30:2025–2032. - PubMed
-
- Broderick JP, Brott TG, Duldner JE, Tomsick T, Huster G. Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30 day mortality. Stroke. 1993;24:987–993. - PubMed
-
- Broderick JP, Brott TG, Tomsick T, Barsan W, Spilker J. Ultra-early evaluation of intracerebral hemorrhage. J Neurosurg. 1990;72:195–199. - PubMed
-
- Brott T, Broderick J, Kothari R, Barsan W, Tomsick T, Sauerbeck L, et al. Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke. 1997;28:1–5. - PubMed
LinkOut - more resources
Full Text Sources

