Serial analysis of imaging parameters in patients with newly diagnosed glioblastoma multiforme
- PMID: 21297128
- PMCID: PMC3093330
- DOI: 10.1093/neuonc/noq194
Serial analysis of imaging parameters in patients with newly diagnosed glioblastoma multiforme
Abstract
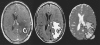
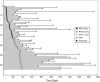
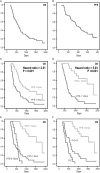
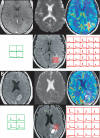
The objective of this study was to test the predictive value of serial MRI data in relation to clinical outcome for patients with glioblastoma multiforme (GBM). Sixty-four patients with newly diagnosed GBM underwent conventional MRI and diffusion-weighted and perfusion-weighted imaging postsurgery and prior to radiation/chemotherapy (pre-RT), immediately after RT (post-RT), and every 1-2 months thereafter until tumor progression, up to a maximum of 1 year. Tumor volumes and perfusion and diffusion parameters were calculated and subject to time-independent and time-dependent Cox proportional hazards models that were adjusted for age and MR scanner field strength. Larger volumes of the T2 hyperintensity lesion (T2ALL) and nonenhancing lesion (NEL) at pre-RT, as well as increased anatomic volumes at post-RT, were associated with worse overall survival (OS). Higher normalized cerebral blood volumes (nCBVs), normalized peak height (nPH) and normalized recirculation factors (nRF) at pre-RT, and nCBV at post-RT, in the T2ALL and NEL, were associated with shorter progression-free survival (PFS). From pre- to post-RT, there was a reduction in nCBV and nPH and an increase in apparent diffusion coefficient (ADC). Patients with lower nRF values at pre-RT, or a larger increase in nRF from pre-RT to post-RT, had significantly longer PFS. Time-dependent analysis showed that patterns of changes in ADC and anatomic volumes were associated with OS, while changes in nCBV, nPH, and the contrast-enhancing volume were associated with PFS. Our studies suggest that quantitative MRI variables derived from anatomic and physiological MRI provide useful information for predicting outcome in patients with GBM.
Figures

References
-
- Stupp R, Mason WP, van den Bent MJ, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005;352:987–996. - PubMed
-
- Macdonald DR, Cascino TL, Schold SC, Jr., Cairncross JG. Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol. 1990;8:1277–1280. - PubMed
-
- Yang I, Aghi MK. New advances that enable identification of glioblastoma recurrence. Nat Rev Clin Oncol. 2009;6:648–657. - PubMed
-
- Burger PC, Green SB. Patient age, histologic features, and length of survival in patients with glioblastoma multiforme. Cancer. 1987;59:1617–1625. - PubMed
-
- Hohwieler Schloss M, Freidberg SR, Heatley GJ, Lo TC. Glucocorticoid dependency as a prognostic factor in radiotherapy for cerebral gliomas. Acta Oncol. 1989;28:51–55. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

