Toward optimization of imaging system and lymphatic tracer for near-infrared fluorescent sentinel lymph node mapping in breast cancer
- PMID: 21360250
- PMCID: PMC3139732
- DOI: 10.1245/s10434-011-1566-x
Toward optimization of imaging system and lymphatic tracer for near-infrared fluorescent sentinel lymph node mapping in breast cancer
Abstract
Background: Near-infrared (NIR) fluorescent sentinel lymph node (SLN) mapping in breast cancer requires optimized imaging systems and lymphatic tracers.
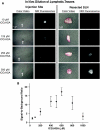
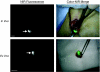
Materials and methods: A small, portable version of the FLARE imaging system, termed Mini-FLARE, was developed for capturing color video and two semi-independent channels of NIR fluorescence (700 and 800 nm) in real time. Initial optimization of lymphatic tracer dose was performed using 35-kg Yorkshire pigs and a 6-patient pilot clinical trial. More refined optimization was performed in 24 consecutive breast cancer patients. All patients received the standard of care using (99m)Technetium-nanocolloid and patent blue. In addition, 1.6 ml of indocyanine green adsorbed to human serum albumin (ICG:HSA) was injected directly after patent blue at the same location. Patients were allocated to 1 of 8 escalating ICG:HSA concentration groups from 50 to 1000 μM.
Results: The Mini-FLARE system was positioned easily in the operating room and could be used up to 13 in. from the patient. Mini-FLARE enabled visualization of lymphatic channels and SLNs in all patients. A total of 35 SLNs (mean = 1.45, range 1-3) were detected: 35 radioactive (100%), 30 blue (86%), and 35 NIR fluorescent (100%). Contrast agent quenching at the injection site and dilution within lymphatic channels were major contributors to signal strength of the SLN. Optimal injection dose of ICG:HSA ranged between 400 and 800 μM. No adverse reactions were observed.
Conclusions: We describe the clinical translation of a new NIR fluorescence imaging system and define the optimal ICG:HSA dose range for SLN mapping in breast cancer.
Trial registration: ClinicalTrials.gov NCT00721370.
Figures

Similar articles
-
Randomized comparison of near-infrared fluorescence imaging using indocyanine green and 99(m) technetium with or without patent blue for the sentinel lymph node procedure in breast cancer patients.Ann Surg Oncol. 2012 Dec;19(13):4104-11. doi: 10.1245/s10434-012-2466-4. Epub 2012 Jul 3. Ann Surg Oncol. 2012. PMID: 22752379 Free PMC article. Clinical Trial.
-
Near Infrared Fluorescent Lymph Node Mapping with Indocyanine Green in Breast Cancer Patients: A Prospective Trial.J Am Coll Surg. 2019 Apr;228(4):672-678. doi: 10.1016/j.jamcollsurg.2018.12.001. Epub 2018 Dec 21. J Am Coll Surg. 2019. PMID: 30582975 Clinical Trial.
-
Clinical trial of combined radio- and fluorescence-guided sentinel lymph node biopsy in breast cancer.Br J Surg. 2013 Jul;100(8):1037-44. doi: 10.1002/bjs.9159. Epub 2013 May 21. Br J Surg. 2013. PMID: 23696463 Free PMC article.
-
Sentinel node mapping with indocyanine green and endoscopic near-infrared fluorescence imaging in endometrial cancer. A pilot study and review of the literature.Gynecol Oncol. 2015 Jun;137(3):443-7. doi: 10.1016/j.ygyno.2015.03.004. Epub 2015 Mar 11. Gynecol Oncol. 2015. PMID: 25771495 Review.
-
Tracers and corresponding detection devices: technetium colloids, blue dyes & NIR fluorescence.Chin Clin Oncol. 2021 Apr;10(2):16. doi: 10.21037/cco-20-252. Chin Clin Oncol. 2021. PMID: 33951916 Review.
Cited by
-
Compact solid-state CMOS single-photon detector array for in vivo NIR fluorescence lifetime oncology measurements.Biomed Opt Express. 2016 Apr 11;7(5):1797-814. doi: 10.1364/BOE.7.001797. eCollection 2016 May 1. Biomed Opt Express. 2016. PMID: 27231622 Free PMC article.
-
Visualization of lymphatic flow in laparoscopic colon cancer surgery using indocyanine green fluorescence imaging.Sci Rep. 2020 Aug 31;10(1):14274. doi: 10.1038/s41598-020-71215-3. Sci Rep. 2020. PMID: 32868829 Free PMC article.
-
Short-term and long-term outcomes of indocyanine green for sentinel lymph node biopsy in early-stage breast cancer.World J Surg Oncol. 2022 Aug 9;20(1):253. doi: 10.1186/s12957-022-02719-7. World J Surg Oncol. 2022. PMID: 35941602 Free PMC article.
-
Quantitative assessment of nipple perfusion with near-infrared fluorescence imaging.Ann Plast Surg. 2013 Feb;70(2):149-53. doi: 10.1097/SAP.0b013e31822f9af7. Ann Plast Surg. 2013. PMID: 21862913 Free PMC article.
-
Intraoperative near-infrared fluorescence imaging of a paraganglioma using methylene blue: A case report.Int J Surg Case Rep. 2015;6C:150-3. doi: 10.1016/j.ijscr.2014.12.002. Epub 2014 Dec 5. Int J Surg Case Rep. 2015. PMID: 25541370 Free PMC article.
References
-
- Krag DN, Anderson SJ, Julian TB, Brown AM, Harlow SP, Ashikaga T, et al. Technical outcomes of sentinel-lymph-node resection and conventional axillary-lymph-node dissection in patients with clinically node-negative breast cancer: results from the NSABP B-32 randomised phase III trial. Lancet Oncol. 2007;8:881–888. doi: 10.1016/S1470-2045(07)70278-4. - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

