Dropping the baton: specialty referrals in the United States
- PMID: 21418312
- PMCID: PMC3160594
- DOI: 10.1111/j.1468-0009.2011.00619.x
Dropping the baton: specialty referrals in the United States
Abstract
Context: In the United States, more than a third of patients are referred to a specialist each year, and specialist visits constitute more than half of outpatient visits. Despite the frequency of referrals and the importance of the specialty-referral process, the process itself has been a long-standing source of frustration among both primary care physicians (PCPs) and specialists. These frustrations, along with a desire to lower costs, have led to numerous strategies to improve the specialty-referral process, such as using gatekeepers and referral guidelines.
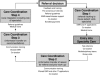
Methods: This article reviews the literature on the specialty-referral process in order to better understand what is known about current problems with the referral process and what solutions have been proposed. The article first provides a conceptual framework and then reviews prior literature on the referral decision, care coordination including information transfer, and access to specialty care.
Findings: PCPs vary in their threshold for referring a patient, which results in both the underuse and the overuse of specialists. Many referrals do not include a transfer of information, either to or from the specialist; and when they do, it often contains insufficient data for medical decision making. Care across the primary-specialty interface is poorly integrated; PCPs often do not know whether a patient actually went to the specialist, or what the specialist recommended. PCPs and specialists also frequently disagree on the specialist's role during the referral episode (e.g., single consultation or continuing co-management).
Conclusions: There are breakdowns and inefficiencies in all components of the specialty-referral process. Despite many promising mechanisms to improve the referral process, rigorous evaluations of these improvements are needed.
© 2011 Milbank Memorial Fund. Published by Wiley Periodicals Inc.
Figures
References
-
- AAFP (American Academy of Family Physicians) Group Visits (Shared Medical Appointments) 2009. Available at http://www.aafp.org/online/en/home/practicemgt/quality/qitools/pracredes... (accessed February 4, 2011)
-
- Akbari A, Mayhew A, Al-Alawi M, Grimshaw JM, Winkens RA, Glidewell E, Pritchard C, Thomas R, Fraser C. Interventions to Improve Outpatient Referrals from Primary Care to Secondary Care. Cochrane Database of Systematic Reviews. 2005 CD005471. - PubMed
-
- Avidor Y, Still CD, Brunner M, Buchwald JN, Buchwald H. Primary Care and Subspecialty Management of Morbid Obesity: Referral Patterns for Bariatric Surgery. Surgery for Obesity and Related Diseases. 2007;3:392–407. - PubMed
-
- Ayanian JZ, Landrum MB, Guadagnoli E, Gaccione P. Specialty of Ambulatory Care Physicians and Mortality among Elderly Patients after Myocardial Infarction. New England Journal of Medicine. 2002;347:1678–86. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical