Merkel cell carcinoma
- PMID: 21422993
- PMCID: PMC3121923
- DOI: 10.1097/COC.0b013e318210f83c
Merkel cell carcinoma
Abstract
Merkel cell carcinoma (MCC) is a rare, clinically aggressive cutaneous neuroendocrine neoplasm with a high mortality rate. Though the etiology is not precisely known, Merkel cell polyomavirus DNA has been found recently in a large percentage of MCC tumors. Other suggested risk factors include sun exposure, immunosuppression, and a history of prior malignancy. Work up of patients with MCC most notably includes nodal staging via clinical examination or sentinel lymph node biopsy. The prognosis for most patients with MCC is poor, and the rarity of MCC precludes the prospective, randomized clinical trials necessary to elucidate optimum treatment protocols. Most published data support the use of a multimodality approach centered around surgical excision with negative margins, sentinel lymph node biopsy to establish the presence or absence of nodal metastases, adjuvant radiothearpy to decrease the risk of recurrence, and systemic chemotherapy in the case of widespread disease.
Figures
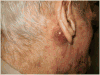




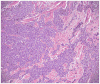



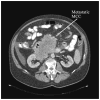



References
-
- Toker C. Trabecular carcinoma of the skin. Arch Dermatol. 1972;105:107–110. - PubMed
-
- Hodgson NC. Merkel cell carcinoma: changing incidence trends. J Surg Oncol. 2005;89:1–4. - PubMed
-
- Goessling W, McKee PH, Mayer RJ. Merkel cell carcinoma. J Clin Oncol. 2002;20:588–598. - PubMed
-
- Merkel F. Tastzellen and Tastkoerperchen bei Den Hausthieren und beim men- schen. Arch Mikrosc Anat. 1875;11:636–652.
-
- Frigerio B, Capella C, Eusebi V, et al. Merkel cell carcinoma of the skin: the structure and origin of normal Merkel cells. Histopathology. 1983;7:229–249. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

