Pulsatile flow into the aqueous veins: manifestations in normal and glaucomatous eyes
- PMID: 21440541
- PMCID: PMC4535453
- DOI: 10.1016/j.exer.2011.03.011
Pulsatile flow into the aqueous veins: manifestations in normal and glaucomatous eyes
Abstract
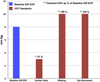
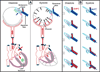
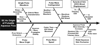
The aqueous outflow system is unique because nowhere else can the pattern of flow of an extravascular fluid be directly observed as it returns to the vascular system. Such observations reveal that aqueous flow both from Schlemm's canal into the aqueous veins and from the aqueous veins into the episcleral veins is pulsatile. Pulsatile aqueous flow mechanisms are observable in vivo not only in normal and but also in glaucomatous eyes. A series of specific patterns accompany the pulsatile mixing of aqueous with blood in the episcleral veins. These directly observable patterns of pulsatile flow are synchronous with intraocular pressure (IOP) transients induced by the cardiac pulse, blinking and eye movement. Patterns of pulsatile flow are altered by events that increase IOP such as pressure on the side of the eye, tonography and water drinking. Pulsatile flow stops when IOP is reduced below its resting level, but begins again when IOP returns to the resting level. Pulsatile flow reduction probably results from the intrinsic reduction of pulse amplitude at a lower IOP, and may thus provide a passive mechanism to maintain short-term homeostasis. Thus modulation of the pulsatile flow phenomenon appears to maintain a homeostatic IOP setpoint. Visible pulsatile flow abnormalities develop in glaucoma patients. Medications that reduce IOP through improvement in outflow do so through pulsatile flow mechanisms. Laboratory studies have demonstrated that cyclic stresses in outflow tissues alter signaling pathways, cytoskeletal responses, extracellular matrix composition and cytokine secretion. How physiologic pulse transients orchestrate cellular responses and how cellular responses identified in the laboratory may in turn regulate pulsatile aqueous outflow is unknown. Linkage of laboratory and in vivo observations await an improved understanding of how cellular and extracellular structures within the outflow system are able to generate an aqueous pulse wave. The purpose of the current report is to provide a summary of in vivo IOP-induced patterns of cyclic flow that can be used as part of a framework for interpretation of responses to cyclic stresses identified in the laboratory.
Copyright © 2011 Elsevier Ltd. All rights reserved.
Figures


Similar articles
-
Aqueous outflow - A continuum from trabecular meshwork to episcleral veins.Prog Retin Eye Res. 2017 Mar;57:108-133. doi: 10.1016/j.preteyeres.2016.12.004. Epub 2016 Dec 24. Prog Retin Eye Res. 2017. PMID: 28028002 Free PMC article. Review.
-
Aqueous outflow regulation: Optical coherence tomography implicates pressure-dependent tissue motion.Exp Eye Res. 2017 May;158:171-186. doi: 10.1016/j.exer.2016.06.007. Epub 2016 Jun 11. Exp Eye Res. 2017. PMID: 27302601 Free PMC article. Review.
-
Aqueous outflow regulation - 21st century concepts.Prog Retin Eye Res. 2021 Jul;83:100917. doi: 10.1016/j.preteyeres.2020.100917. Epub 2020 Nov 17. Prog Retin Eye Res. 2021. PMID: 33217556 Free PMC article. Review.
-
The aqueous outflow system as a mechanical pump: evidence from examination of tissue and aqueous movement in human and non-human primates.J Glaucoma. 2004 Oct;13(5):421-38. doi: 10.1097/01.ijg.0000131757.63542.24. J Glaucoma. 2004. PMID: 15354083 Review.
-
The Effects of Trabecular Bypass Surgery on Conventional Aqueous Outflow, Visualized by Hemoglobin Video Imaging.J Glaucoma. 2020 Aug;29(8):656-665. doi: 10.1097/IJG.0000000000001561. J Glaucoma. 2020. PMID: 32773669
Cited by
-
Tissue-Engineered Models for Glaucoma Research.Micromachines (Basel). 2020 Jun 24;11(6):612. doi: 10.3390/mi11060612. Micromachines (Basel). 2020. PMID: 32599818 Free PMC article. Review.
-
Conjunctival and Intrascleral Vasculatures Assessed Using Anterior Segment Optical Coherence Tomography Angiography in Normal Eyes.Am J Ophthalmol. 2018 Dec;196:1-9. doi: 10.1016/j.ajo.2018.08.009. Epub 2018 Aug 9. Am J Ophthalmol. 2018. PMID: 30099035 Free PMC article.
-
Transient Intraocular Pressure Fluctuations: Source, Magnitude, Frequency, and Associated Mechanical Energy.Invest Ophthalmol Vis Sci. 2019 Jun 3;60(7):2572-2582. doi: 10.1167/iovs.19-26600. Invest Ophthalmol Vis Sci. 2019. PMID: 31212310 Free PMC article.
-
Intraocular pressure homeostasis: maintaining balance in a high-pressure environment.J Ocul Pharmacol Ther. 2014 Mar-Apr;30(2-3):94-101. doi: 10.1089/jop.2013.0185. Epub 2014 Jan 8. J Ocul Pharmacol Ther. 2014. PMID: 24401029 Free PMC article. Review.
-
Isolation and characterization of novel primary cells from the human distal outflow pathway.Sci Rep. 2021 Feb 17;11(1):4034. doi: 10.1038/s41598-021-83558-6. Sci Rep. 2021. PMID: 33597641 Free PMC article.
References
-
- Ascher KW. Aqueous veins: preliminary note. Am. J. Ophthalmol. 1942a;25:31–38.
-
- Ascher KW. Local pharmacologic effects on aqueous veins. Am. J. Ophthalmol. 1942b;25:1301–1315.
-
- Ascher KW. Physiologic importance of the visible elimination of intraocular fluid. Am. J. Ophthalmol. 1942c;25:1174–1209. - PubMed
-
- Ascher KW. Glaucoma and the aqueous veins. Am. J. Ophthalmol. 1942d;25:1309–1315.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

