Allergen-specific subcutaneous immunotherapy in allergic asthma: immunologic mechanisms and improvement
- PMID: 21483568
- PMCID: PMC3071166
- DOI: 10.3402/ljm.v5i0.5303
Allergen-specific subcutaneous immunotherapy in allergic asthma: immunologic mechanisms and improvement
Abstract
Allergic asthma is a disease characterized by persistent allergen-driven airway inflammation, remodeling, and airway hyperresponsiveness. CD4(+) T-cells, especially T-helper type 2 cells, play a critical role in orchestrating the disease process through the release of the cytokines IL-4, IL-5, and IL-13. Allergen-specific immunotherapy (SIT) is currently the only treatment with a long-term effect via modifying the natural course of allergy by interfering with the underlying immunological mechanisms. However, although SIT is effective in allergic rhinitis and insect venom allergy, in allergic asthma it seldom results in complete alleviation of the symptoms. Improvement of SIT is needed to enhance its efficacy in asthmatic patients. Herein, the immunoregulatory mechanisms underlying the beneficial effects of SIT are discussed with the ultimate aim to improve its treatment efficacy.
Keywords: IL-10; IgE; Th2 lymphocytes; allergic asthma; dendritic cell; eosinophilia; hyperresponsiveness; immunotherapy; regulatory T cells.
Figures

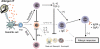
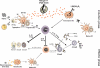
References
-
- Maddox L, Schwartz DA. The pathophysiology of asthma. Annu Rev Med. 2002;53:477–98. - PubMed
-
- EUROP WHO. Environmental hazards trigger childhood allergic disorders. Fact sheet EURO/01/3. 2003 Apr
-
- Bosse Y, Hudson TJ. Toward a comprehensive set of asthma susceptibility genes. Annu Rev Med. 2007;58:171–84. - PubMed
-
- Carroll W. Asthma genetics: pitfalls and triumphs. Paediatr Respir Rev. 2005;6:68–74. - PubMed
-
- Cookson WO. Asthma genetics. Chest. 2002;121:S7–S13. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
