Population density, call-response interval, and survival of out-of-hospital cardiac arrest
- PMID: 21489299
- PMCID: PMC3100230
- DOI: 10.1186/1476-072X-10-26
Population density, call-response interval, and survival of out-of-hospital cardiac arrest
Abstract
Background: Little is known about the effects of geographic variation on outcomes of out-of-hospital cardiac arrest (OHCA). The present study investigated the relationship between population density, time between emergency call and ambulance arrival, and survival of OHCA, using the All-Japan Utstein-style registry database, coupled with geographic information system (GIS) data.
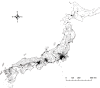
Methods: We examined data from 101,287 bystander-witnessed OHCA patients who received emergency medical services (EMS) through 4,729 ambulatory centers in Japan between 2005 and 2007. Latitudes and longitudes of each center were determined with address-match geocoding, and linked with the Population Census data using GIS. The endpoints were 1-month survival and neurologically favorable 1-month survival defined as Glasgow-Pittsburgh cerebral performance categories 1 or 2.
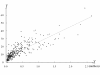
Results: Overall 1-month survival was 7.8%. Neurologically favorable 1-month survival was 3.6%. In very low-density (<250/km(2)) and very high-density (≥10,000/km(2)) areas, the mean call-response intervals were 9.3 and 6.2 minutes, 1-month survival rates were 5.4% and 9.1%, and neurologically favorable 1-month survival rates were 2.7% and 4.3%, respectively. After adjustment for age, sex, cause of arrest, first aid by bystander and the proportion of neighborhood elderly people ≥65 yrs, patients in very high-density areas had a significantly higher survival rate (odds ratio (OR), 1.64; 95% confidence interval (CI), 1.44 - 1.87; p < 0.001) and neurologically favorable 1-month survival rate (OR, 1.47; 95%CI, 1.22 - 1.77; p < 0.001) compared with those in very low-density areas.
Conclusion: Living in a low-density area was associated with an independent risk of delay in ambulance response, and a low survival rate in cases of OHCA. Distribution of EMS centers according to population size may lead to inequality in health outcomes between urban and rural areas.
Figures

Similar articles
-
Citizen bystander-patient relationship and 1-month outcomes after out-of-hospital cardiac arrest of cardiac origin from the All-Japan Utstein Registry: a prospective, nationwide, population-based, observational study.BMJ Open. 2019 Jul 26;9(7):e024715. doi: 10.1136/bmjopen-2018-024715. BMJ Open. 2019. PMID: 31350237 Free PMC article.
-
Out-of-hospital cardiac arrest surveillance --- Cardiac Arrest Registry to Enhance Survival (CARES), United States, October 1, 2005--December 31, 2010.MMWR Surveill Summ. 2011 Jul 29;60(8):1-19. MMWR Surveill Summ. 2011. PMID: 21796098
-
Relationship Between Emergency Medical Services Response Time and Bystander Intervention in Patients With Out-of-Hospital Cardiac Arrest.J Am Heart Assoc. 2018 Apr 27;7(9):e007568. doi: 10.1161/JAHA.117.007568. J Am Heart Assoc. 2018. PMID: 29703811 Free PMC article.
-
Effects of prehospital epinephrine administration on neurologically intact survival in bystander-witnessed out-of-hospital cardiac arrest patients with non-shockable rhythm depend on prehospital cardiopulmonary resuscitation duration required to hospital arrival.Heart Vessels. 2018 Dec;33(12):1525-1533. doi: 10.1007/s00380-018-1205-6. Epub 2018 Jun 23. Heart Vessels. 2018. PMID: 29936632
-
Community first responders for out-of-hospital cardiac arrest in adults and children.Cochrane Database Syst Rev. 2019 Jul 19;7(7):CD012764. doi: 10.1002/14651858.CD012764.pub2. Cochrane Database Syst Rev. 2019. PMID: 31323120 Free PMC article.
Cited by
-
Increased number of dispatches in emergency medical services correlates to response time extension.Acute Med Surg. 2024 Nov 5;11(1):e70017. doi: 10.1002/ams2.70017. eCollection 2024 Jan-Dec. Acute Med Surg. 2024. PMID: 39503016 Free PMC article.
-
Spatial decision on allocating automated external defibrillators (AED) in communities by multi-criterion two-step floating catchment area (MC2SFCA).Int J Health Geogr. 2016 May 25;15(1):17. doi: 10.1186/s12942-016-0046-8. Int J Health Geogr. 2016. PMID: 27225882 Free PMC article.
-
A validation of ground ambulance pre-hospital times modeled using geographic information systems.Int J Health Geogr. 2012 Oct 3;11:42. doi: 10.1186/1476-072X-11-42. Int J Health Geogr. 2012. PMID: 23033894 Free PMC article.
-
Factors modifying performance of a novel citizen text message alert system in improving survival of out-of-hospital cardiac arrest.Eur Heart J Acute Cardiovasc Care. 2018 Aug;7(5):397-404. doi: 10.1177/2048872617694675. Epub 2017 Mar 13. Eur Heart J Acute Cardiovasc Care. 2018. PMID: 28635305 Free PMC article.
-
Subsequent Shockable Rhythm During Out-of-Hospital Cardiac Arrest in Children With Initial Non-Shockable Rhythms: A Nationwide Population-Based Observational Study.J Am Heart Assoc. 2016 Oct 17;5(10):e003589. doi: 10.1161/JAHA.116.003589. J Am Heart Assoc. 2016. PMID: 27792647 Free PMC article.
References
-
- Yasunaga H, Horiguchi H, Tanabe S, Akahane M, Ogawa T, Koike S, Imamura T. Collaborative effects of bystander-initiated cardiopulmonary resuscitation and prehospital advanced cardiac life support by physicians on survival of out-of-hospital cardiac arrest: a nationwide population-based observational study. Crit Care. 2010;14:R199. doi: 10.1186/cc9319. - DOI - PMC - PubMed
-
- Stiell IG, Wells GA, Field B, Spaite DW, Nesbitt LP, De Maio VJ, Nichol G, Cousineau D, Blackburn J, Munkley D, Luinstra-Toohey L, Campeau T, Dagnone E, Lyver M. Advanced cardiac life support in out-of-hospital cardiac arrest. N Engl J Med. 2004;351:647–656. doi: 10.1056/NEJMoa040325. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

