Temporal and Geographic variation in the validity and internal consistency of the Nursing Home Resident Assessment Minimum Data Set 2.0
- PMID: 21496257
- PMCID: PMC3097253
- DOI: 10.1186/1472-6963-11-78
Temporal and Geographic variation in the validity and internal consistency of the Nursing Home Resident Assessment Minimum Data Set 2.0
Abstract
Background: The Minimum Data Set (MDS) for nursing home resident assessment has been required in all U.S. nursing homes since 1990 and has been universally computerized since 1998. Initially intended to structure clinical care planning, uses of the MDS expanded to include policy applications such as case-mix reimbursement, quality monitoring and research. The purpose of this paper is to summarize a series of analyses examining the internal consistency and predictive validity of the MDS data as used in the "real world" in all U.S. nursing homes between 1999 and 2007.
Methods: We used person level linked MDS and Medicare denominator and all institutional claim files including inpatient (hospital and skilled nursing facilities) for all Medicare fee-for-service beneficiaries entering U.S. nursing homes during the period 1999 to 2007. We calculated the sensitivity and positive predictive value (PPV) of diagnoses taken from Medicare hospital claims and from the MDS among all new admissions from hospitals to nursing homes and the internal consistency (alpha reliability) of pairs of items within the MDS that logically should be related. We also tested the internal consistency of commonly used MDS based multi-item scales and examined the predictive validity of an MDS based severity measure viz. one year survival. Finally, we examined the correspondence of the MDS discharge record to hospitalizations and deaths seen in Medicare claims, and the completeness of MDS assessments upon skilled nursing facility (SNF) admission.
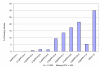
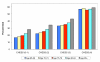
Results: Each year there were some 800,000 new admissions directly from hospital to US nursing homes and some 900,000 uninterrupted SNF stays. Comparing Medicare enrollment records and claims with MDS records revealed reasonably good correspondence that improved over time (by 2006 only 3% of deaths had no MDS discharge record, only 5% of SNF stays had no MDS, but over 20% of MDS discharges indicating hospitalization had no associated Medicare claim). The PPV and sensitivity levels of Medicare hospital diagnoses and MDS based diagnoses were between .6 and .7 for major diagnoses like CHF, hypertension, diabetes. Internal consistency, as measured by PPV, of the MDS ADL items with other MDS items measuring impairments and symptoms exceeded .9. The Activities of Daily Living (ADL) long form summary scale achieved an alpha inter-consistency level exceeding .85 and multi-item scale alpha levels of .65 were achieved for well being and mood, and .55 for behavior, levels that were sustained even after stratification by ADL and cognition. The Changes in Health, End-stage disease and Symptoms and Signs (CHESS) index, a summary measure of frailty was highly predictive of one year survival.
Conclusion: The MDS demonstrates a reasonable level of consistency both in terms of how well MDS diagnoses correspond to hospital discharge diagnoses and in terms of the internal consistency of functioning and behavioral items. The level of alpha reliability and validity demonstrated by the scales suggest that the data can be useful for research and policy analysis. However, while improving, the MDS discharge tracking record should still not be used to indicate Medicare hospitalizations or mortality. It will be important to monitor the performance of the MDS 3.0 with respect to consistency, reliability and validity now that it has replaced version 2.0, using these results as a baseline that should be exceeded.
Figures

References
-
- Morris JN, Hawes C, Fries BE, Phillips CD, Mor V, Katz S, Murphy K, Drugovich ML, Friedlob AS. Designing the national resident assessment instrument for nursing homes. Gerontologist. 1990;30(3):293–307. - PubMed
-
- Mor V. A comprehensive clinical assessment tool to inform policy and practice: applications of the minimum data set. Med Care. 2004;42(4 Suppl):III50–59. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

