Adult peripheral nerve disorders: nerve entrapment, repair, transfer, and brachial plexus disorders
- PMID: 21532404
- PMCID: PMC3864586
- DOI: 10.1097/PRS.0b013e31820cf556
Adult peripheral nerve disorders: nerve entrapment, repair, transfer, and brachial plexus disorders
Abstract
Learning objectives: After reading this article, the participant should be able to: 1. Describe the pathophysiologic bases for nerve injury and how they apply to patient evaluation and management. 2. Recognize the wide variety of injury patterns and associated patient complaints and physical findings associated with peripheral nerve pathology. 3. Evaluate and recommend further tests to aid in defining the diagnosis. 4. Specify treatment options and potential risks and benefits.
Summary: Peripheral nerve disorders comprise a gamut of problems, ranging from entrapment neuropathy to direct open traumatic injury and closed brachial plexus injury. The pathophysiology of injury defines the patient's symptoms, examination findings, and treatment options and is critical to accurate diagnosis and treatment. The goals of treatment include management of the often associated pain and improvement of sensory and motor function. Understanding peripheral nerve anatomy is critical to adopting novel nerve transfer procedures, which may provide superior options for a variety of injury patterns.
Figures

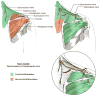
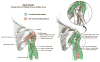
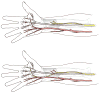

References
-
- Mackinnon SE, Dellon AL. Surgery of the Peripheral Nerve. New York: Thieme Medical Publishers, Inc; 1988.
-
- Sunderland S. A classification of peripheral nerve injuries producing loss of function. Brain. 1951;74:491–516. - PubMed
-
- Mackinnon SE, Novak CB. Compression Neuropathies. In: Green DP, Hotchkiss RN, Pederson WC, et al., editors. Green’s Operative Hand Surgery. 5. Vol. 1. Philadelphia: Elsevier, Inc; 2005. pp. 999–1045.
-
- Strauch B, Lang A. The ten test revisited. Plast Reconstr Surg. 2003;112:593–594. - PubMed
-
- Strauch B, Lang A, Ferder M, et al. The ten test. Plast Reconstr Surg. 1997;99:1074–1078. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

