Impact of transarterial therapy in hepatitis C-related hepatocellular carcinoma on long-term outcomes after liver transplantation
- PMID: 21552101
- PMCID: PMC3155640
- DOI: 10.1097/COC.0b013e31821631f6
Impact of transarterial therapy in hepatitis C-related hepatocellular carcinoma on long-term outcomes after liver transplantation
Abstract
Objectives: To evaluate the impact of long-term outcomes of transarterial embolization (TAE) therapy in patients with hepatitis C virus (HCV)-related hepatocellular carcinoma (HCC) on the waiting list for liver transplantation (LT).
Methods: We retrospectively evaluated the post-LT patients with HCV-related HCC who received TAE intervention (n=33) and those who had no treatment (n=47) while on the waiting list to determine long-term outcomes.
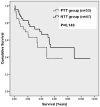
Results: Over a 10-year period, of the 424 patients transplanted with HCV, 80 patients had HCC with a tumor burden within Milan criteria. For the entire study cohort, the mean duration of post-LT follow-up was 3.5 years; mean time of transplant waiting list was 120 days; and median post-LT survival was 8.9 years. The survival rates at 1, 3, 5, and 10 years were 82%, 70%, 55%, and 35%, respectively. From the study cohort, 33 patients received TAE and 47 patients did not while on the waiting list. The 2 groups were well matched, except, that the intervention patients received post-LT interferon more often and had a shorter time on the waiting list (56.2 d) when compared with the no treatment group (164.6 d, P<0.001). Median survival in the TAE group was 4.8 years and 8.9 years in the no treatment group. The recurrence rate was 15.6% in the treatment group and 6.9% in the no therapy group (P=0.275).
Conclusions: Pre-LT transarterial therapy has no benefit on post-LT survival and tumor recurrence in patients with HCV-related HCC who underwent a mean waiting period of <3 months to transplant.
Figures
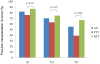
References
-
- Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, 2002. CA Cancer J Clin. 2005 Mar;55(2):74–108. - PubMed
-
- Jemal A, Murray T, Ward E, Samuels A, Tiwari RC, Ghafoor A, et al. Cancer statistics, 2005. CA Cancer J Clin. 2005 Jan;55(1):10–30. - PubMed
-
- El-Serag HB, Rudolph KL. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology. 2007 Jun;132(7):2557–76. Review. - PubMed
-
- Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003 Apr 24;348(17):1625–38. - PubMed
-
- El-Serag HB, Tran T, Everhart JE. Diabetes increases the risk of chronic liver disease and hepatocellular carcinoma. Gastroenterology. 2004 Feb;126(2):460–8. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

