Differential effects of HIV viral load and CD4 count on proliferation of naive and memory CD4 and CD8 T lymphocytes
- PMID: 21562041
- PMCID: PMC3138680
- DOI: 10.1182/blood-2011-02-335174
Differential effects of HIV viral load and CD4 count on proliferation of naive and memory CD4 and CD8 T lymphocytes
Abstract
We previously showed that HIV infection leads to expansion of a rapidly proliferating pool (s(1)) of CD4 and CD8 T lymphocytes. In the current study, we used in vivo labeling with bromodeoxyuridine to characterize the kinetics of naive, memory, and activated (HLA-DR(+)/CD38(+)) subpopulations of CD4 and CD8 T lymphocytes, and to examine the relationship between kinetic parameters and baseline CD4 counts, HIV viral load, potential markers of microbial translocation, and cytokine levels. Activated cells showed the highest proliferation rates, followed by effector and central memory cells, with naive cells showing the lowest rates, for both CD4 and CD8 T cells. HIV viral load correlated with s(1) of CD4 and CD8 effector memory cells, as well as CD8 naive cells, whereas CD4 cell counts correlated inversely with naive CD4 s(1). Endotoxin levels showed a weak negative association with CD4 but not CD8 s(1). INF-γ and TNF-α were associated with s(1) for CD4 and CD8 cells, respectively. Thus, HIV is the primary driving force behind the activation and proliferation of most subsets of both CD4 and CD8 T lymphocytes, whereas naive CD4 cell proliferation likely represents a homeostatic response. Microbial translocation does not appear to play an important role in this proliferation.
Figures
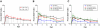



References
-
- Hazenberg MD, Stuart JW, Otto SA, et al. T-cell division in human immunodeficiency virus (HIV)-1 infection is mainly due to immune activation: a longitudinal analysis in patients before and during highly active antiretroviral therapy (HAART). Blood. 2000;95(1):249–255. - PubMed
-
- Giorgi JV, Hultin LE, McKeating JA, et al. Shorter survival in advanced human immunodeficiency virus type 1 infection is more closely associated with T lymphocyte activation than with plasma virus burden or virus chemokine coreceptor usage. J Infect Dis. 1999;179(4):859–870. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

