Bioenergetics, mitochondria, and cardiac myocyte differentiation
- PMID: 21603067
- PMCID: PMC3096664
- DOI: 10.1016/j.ppedcard.2011.02.002
Bioenergetics, mitochondria, and cardiac myocyte differentiation
Abstract
Cardiac metabolism is finely tuned, and disruption of myocardial bioenergetics can be clinically devastating. Many cardiomyopathies that present early in life are due to disruption of the maturation of these metabolic pathways. However, this bioenergetic maturation begins well before birth, when the embryonic heart is first beginning to beat, and continues into the mature animal. Thus, the changes in energy production seen after birth are actually part of a continuum that coincides with the structural and functional changes that occur as the cardiac myocyte differentiates and the heart undergoes morphogenesis. Therefore, although bioenergetics and mitochondrial biology have not been studied in great detail in the developing heart, bioenergetic maturation should be considered an important component of normal myocyte differentiation.Although events occurring after birth will be discussed, this review will focus on the changes in bioenergetics and mitochondrial biology that coincide with myocyte differentiation and cardiac morphogenesis. The relationship of these changes to the etiology and presentation of cardiomyopathies will be used as a starting point for this discussion. Then, after reviewing cardiac development and mitochondrial biology, the published data on bioenergetics and mitochondrial structure and function in the developing heart will be presented. Finally, the case will be made that mitochondria may be critical regulators of cardiac myocyte differentiation and cardiac development.
Figures
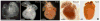



References
-
- Conway SJ, Kruzynska-Frejtag A, Kneer PL, Machnicki M, Koushik SV. What cardiovascular defect does my prenatal mouse mutant have, and why? Genesis. 2003;35:1–21. - PubMed
-
- Turgeon B, Meloche S. Interpreting neonatal lethal phenotypes in mouse mutants: insights into gene function and human diseases. Physiol Rev. 2009;89:1–26. - PubMed
-
- Lipshultz SE, Sleeper LA, Towbin JA, et al. The incidence of pediatric cardiomyopathy in two regions of the United States. N Engl J Med. 2003;348:1647–55. - PubMed
-
- Nugent AW, Daubeney PE, Chondros P, et al. The epidemiology of childhood cardiomyopathy in Australia. N Engl J Med. 2003;348:1639–46. - PubMed
-
- Kelly DP, Strauss AW. Inherited cardiomyopathies. N Engl J Med. 1994;330:913–19. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
