Comparison of genetic and clinical aspects in patients with acute myeloid leukemia and myelodysplastic syndromes all with more than 50% of bone marrow erythropoietic cells
- PMID: 21606170
- PMCID: PMC3166098
- DOI: 10.3324/haematol.2011.043687
Comparison of genetic and clinical aspects in patients with acute myeloid leukemia and myelodysplastic syndromes all with more than 50% of bone marrow erythropoietic cells
Abstract
Background: The World Health Organization separates acute erythroid leukemia (erythropoiesis in ≥50% of nucleated bone marrow cells; ≥20% myeloblasts of non-erythroid cells) from other entities with increased erythropoiesis - acute myeloid leukemia with myelodysplasia-related changes (≥20% myeloblasts of all nucleated cells) or myelodysplastic syndromes - and subdivides acute erythroid leukemia into erythroleukemia and pure erythroid leukemia subtypes. We aimed to investigate the biological/genetic justification for the different categories of myeloid malignancies with increased erythropoiesis (≥50% of bone marrow cells).
Design and methods: We investigated 212 patients (aged 18.5-88.4 years) with acute myeloid leukemia or myelodysplastic syndromes characterized by 50% or more erythropoiesis: 108 had acute myeloid leukemia (77 with acute erythroid leukemia, corresponding to erythroid/myeloid erythroleukemia, 7 with pure erythroid leukemia, 24 with acute myeloid leukemia with myelodysplasia-related changes) and 104 had myelodysplastic syndromes. Morphological and chromosome banding analyses were performed in all cases; subsets of cases were analyzed by polymerase chain reaction and immunophenotyping.
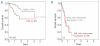
Results: Unfavorable karyotypes were more frequent in patients with acute myeloid leukemia than in those with myelodysplastic syndromes (42.6% versus 13.5%; P<0.0001), but their frequency did not differ significantly between patients with acute erythroid leukemia (39.0%), pure erythroid leukemia (57.1%), and acute myeloid leukemia with myelodysplasia-related changes (50.0%). The incidence of molecular mutations did not differ significantly between the different categories. The 2-year overall survival rate was better for patients with myelodysplastic syndromes than for those with acute myeloid leukemia (P<0.0001), without significant differences across the different acute leukemia subtypes. The 2-year overall survival rate was worse in patients with unfavorable karyotypes than in those with intermediate risk karyotypes (P<0.0001). In multivariate analysis, only myelodysplastic syndromes versus acute myeloid leukemia (P=0.021) and cytogenetic risk category (P=0.002) had statistically significant effects on overall survival.
Conclusions: The separation of acute myeloid leukemia and myelodysplastic syndromes with 50% or more erythropoietic cells has clinical relevance, but it might be worth discussing whether to replace the subclassifications of different subtypes of acute erythroid leukemia and acute myeloid leukemia with myelodysplasia-related changes by the single entity, acute myeloid leukemia with increased erythropoiesis ≥50%.
Figures




Comment in
-
Acute myeloid leukemia with expanded erythropoiesis.Haematologica. 2011 Sep;96(9):1241-3. doi: 10.3324/haematol.2011.050526. Haematologica. 2011. PMID: 21880638 Free PMC article. No abstract available.
References
-
- Arber DA, Brunning RD, Orazi A, Porwit A, Peterson L, Thiele J, et al. Acute myeloid leukemia, not otherwise specified. In: Swerdlow S, Campo E, Harris N, Jaffe E, Pileri S, Stein H, et al., editors. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissue. 4th ed. Lyon: IARC Press; 2008. pp. 130–9.
-
- Fouillard L, Labopin M, Gorin NC, Polge E, Prentice HG, Meloni, et al. Hematopoietic stem cell transplantation for de novo erythroleukemia: a study of the European Group for Blood and Marrow Transplantation (EBMT) Blood. 2002;100(9):3135–40. - PubMed
-
- Arber DA, Brunning RD, Orazi A, Bain BJ, Porwit A, Vardiman JW, et al. Acute myeloid leukaemia with myelodysplasia-related changes. In: Swerdlow S, Campo E, Harris N, Jaffe E, Pileri S, Stein H, et al., editors. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissue. 4th ed. Lyon: IARC Press; 2008. pp. 124–6.
-
- Swerdlow S, Campo E, Lee Harris N, Jaffe E, Pileri S, Stein H, et al. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. 4th ed. Lyon: IARC press; 2008.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

