Progression of cognitive, functional, and neuropsychiatric symptom domains in a population cohort with Alzheimer dementia: the Cache County Dementia Progression study
- PMID: 21606896
- PMCID: PMC3101372
- DOI: 10.1097/JGP.0b013e3181faec23
Progression of cognitive, functional, and neuropsychiatric symptom domains in a population cohort with Alzheimer dementia: the Cache County Dementia Progression study
Abstract
Objectives: Progression of Alzheimer dementia (AD) is highly variable. Most estimates derive from convenience samples from dementia clinics or research centers where there is substantial potential for survival bias and other distortions. In a population-based sample of incident AD cases, we examined progression of impairment in cognition, function, and neuropsychiatric symptoms, and the influence of selected variables on these domains.
Design: Longitudinal, prospective cohort study.
Setting: Cache County (Utah).
Participants: Three hundred twenty-eight persons with a diagnosis of possible/probable AD.
Measurements: Mini-Mental State Exam (MMSE), Clinical Dementia Rating sum-of-boxes (CDR-sb), and Neuropsychiatric Inventory (NPI).
Results: Over a mean follow-up of 3.80 (range: 0.07-12.90) years, the mean (SD) annual rates of change were -1.53 (2.69) scale points on the MMSE, 1.44 (1.82) on the CDR-sb, and 2.55 (5.37) on the NPI. Among surviving participants, 30% to 58% progressed less than 1 point per year on these measures, even 5 to 7 years after dementia onset. Rates of change were correlated between MMSE and CDR-sb (r = -0.62, df = 201, p < 0.001) and between the CDR-sb and NPI (r = 0.20, df = 206, p < 0.004). Female subjects (LR χ = 8.7, df = 2, p = 0.013) and those with younger onset (likelihood ratio [LR] χ = 5.7, df = 2, p = 0.058) declined faster on the MMSE. Although one or more apolipoprotein E ε 4 alleles and ever use of FDA-approved antidementia medications were associated with initial MMSE scores, neither was related to the rate of progression in any domain.
Conclusions: A significant proportion of persons with AD progresses slowly. The results underscore differences between population-based versus clinic-based samples and suggest ongoing need to identify factors that may slow the progression of AD.
Figures
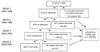

References
-
- Brookmeyer R, Johnson E, Ziegler-Graham K, et al. Forecasting the global burden of Alzheimer's disease. Alzheimers Dement. 2007;3:186–191. - PubMed
-
- Behl P, Stefurak TL, Black SE. Progress in clinical neurosciences: cognitive markers of progression in Alzheimer's disease. The Canadian journal of neurological sciences. 2005;32:140–151. - PubMed
-
- Aguero-Torres H, Fratiglioni L, Winblad B. Natural history of Alzheimer's disease and other dementias: review of the literature in the light of the findings from the Kungsholmen Project. Int J Geriatr Psychiatry. 1998;13:755–766. - PubMed
-
- Chung JA, Cummings JL. Neurobehavioral and neuropsychiatric symptoms in Alzheimer's disease: characteristics and treatment. Neurologic clinics. 2000;18:829–846. - PubMed
-
- Kokmen E, Ozsarfati Y, Beard CM, et al. Impact of referral bias on clinical and epidemiological studies of Alzheimer's disease. Journal of clinical epidemiology. 1996;49:79–83. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- P30 AG028377/AG/NIA NIH HHS/United States
- T32 AG027668/AG/NIA NIH HHS/United States
- R01AG18712/AG/NIA NIH HHS/United States
- K24AG027841/AG/NIA NIH HHS/United States
- P30 AG013846/AG/NIA NIH HHS/United States
- R01HG02213/HG/NHGRI NIH HHS/United States
- R01AG-21136/AG/NIA NIH HHS/United States
- K24 AG027841/AG/NIA NIH HHS/United States
- P30AG13846/AG/NIA NIH HHS/United States
- R01 AG021136/AG/NIA NIH HHS/United States
- R01 AG018712/AG/NIA NIH HHS/United States
- R01 HG002213/HG/NHGRI NIH HHS/United States
- R01AG11380/AG/NIA NIH HHS/United States
- R01 AG011380/AG/NIA NIH HHS/United States
- P30AG028377/AG/NIA NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

