Clinical value of prognostic instruments to identify patients with an increased risk for osteoporotic fractures: systematic review
- PMID: 21625596
- PMCID: PMC3097232
- DOI: 10.1371/journal.pone.0019994
Clinical value of prognostic instruments to identify patients with an increased risk for osteoporotic fractures: systematic review
Erratum in
- PLoS One. 2011;6(8). doi:10.1371/annotation/7596ad0d-c602-4e5f-a7ae-caf7d5802720
Abstract
Background: With the broad availability of effective medications, identifying individuals bearing a higher risk for osteoporotic fractures has become an issue of major concern in modern medicine. In recent years various prognostic instruments have become available showing conflicting results regarding estimated risks for individual patients.
Objective: To provide an overview of current evidence and of opportunities for further research.
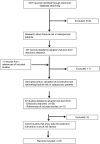
Methodology/principal findings: Systematic review: We identified studies describing the development of instruments and all subsequent validations in electronic databases and reference lists of included studies. We screened for inclusion, read full papers and extracted data on salient clinical features, performance characteristics and quality in duplicate. Searches retrieved 5,275 records of which full texts of 167 papers were obtained after screening titles and abstract. We included 35 studies enrolling a total of 609,969 patients (median 2546) reporting on 31 derivations and 12 validations after assessing full texts. Median follow-up time was 4.1 years (IQR 3 to 7.7). Only four studies validated an instrument that was developed by another group. None of the existing instruments was validated more than once. The five most frequent included variables in the final model were age, body mass index, bone mass index, past history of falls, and maternal history of fractures. The methodological quality of the studies was moderate.
Conclusion: There is a plethora of evidence available studying the association of risk profiles and the development of osteoporotic fractures. The small number of out-of-sample validations, the large variety of study characteristics, outcomes and follow-up periods impedes from deriving robust summaries and from conclusions regarding the clinical performance of many tools. First and foremost, future activity in this field should aim at reaching a consensus among clinical experts in respect to the existing instruments. Then we call for careful validations and expedient adaptations for local circumstances of the most promising candidates.
Conflict of interest statement
References
-
- Lippuner K, Johansson H, Kanis JA, Rizzoli R. Remaining lifetime and absolute 10-year probabilities of osteoporotic fracture in Swiss men and women. Osteoporos Int. 2009;20:1131–1140. - PubMed
-
- Wainwright SA, Marshall LM, Ensrud KE, Cauley JA, Black DM, et al. Hip fracture in women without osteoporosis. J Clin Endocrinol Metab. 2005;90:2787–2793. - PubMed
-
- Albrand G, Munoz F, Sornay RE, DuBoeuf F, Delmas PD. Independent predictors of all osteoporosis-related fractures in healthy postmenopausal women: The OFELY Study. Bone. 2003;32:78–85. - PubMed
-
- Barrett CE, Siris ES, Wehren LE, Miller PD, Abbott TA, et al. Osteoporosis and fracture risk in women of different ethnic groups. Journal of Bone and Mineral Research. 2005;20:185–194. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous