Pulmonary alveolar proteinosis
- PMID: 21632797
- PMCID: PMC9487789
- DOI: 10.1183/09059180.00001311
Pulmonary alveolar proteinosis
Abstract
Pulmonary alveolar proteinosis (PAP) is a rare pulmonary disease characterised by alveolar accumulation of surfactant. It may result from mutations in surfactant proteins or granulocyte macrophage-colony stimulating factor (GM-CSF) receptor genes, it may be secondary to toxic inhalation or haematological disorders, or it may be auto-immune, with anti-GM-CSF antibodies blocking activation of alveolar macrophages. Auto-immune alveolar proteinosis is the most frequent form of PAP, representing 90% of cases. Although not specific, high-resolution computed tomography shows a characteristic "crazy paving" pattern. In most cases, bronchoalveolar lavage findings establish the diagnosis. Whole lung lavage is the most effective therapy, especially for auto-immune disease. Novel therapies targeting alveolar macrophages (recombinant GM-CSF therapy) or anti-GM-CSF antibodies (rituximab and plasmapheresis) are being investigated. Our knowledge of the pathophysiology of PAP has improved in the past 20 yrs, but therapy for PAP still needs improvement.
Conflict of interest statement
None declared.
Figures
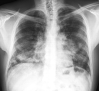




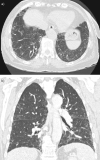
Comment in
-
The milky (path)way of proteinosis: has the time come.Eur Respir Rev. 2011 Jun;20(120):67-8. doi: 10.1183/09059180.00003011. Eur Respir Rev. 2011. PMID: 21632793 Free PMC article. No abstract available.
References
-
- Dranoff G, Crawford AD, Sadelain M, et al. . Involvement of granulocyte-macrophage colony-stimulating factor in pulmonary homeostasis. Science 1994; 264: 713–716. - PubMed
-
- Shibata Y, Berclaz PY, Chroneos ZC, et al. . GM-CSF regulates alveolar macrophage differentiation and innate immunity in the lung through PU.1. Immunity 2001; 15: 557–567. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous
