Perishock pause: an independent predictor of survival from out-of-hospital shockable cardiac arrest
- PMID: 21690495
- PMCID: PMC3138806
- DOI: 10.1161/CIRCULATIONAHA.110.010736
Perishock pause: an independent predictor of survival from out-of-hospital shockable cardiac arrest
Abstract
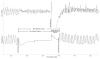
Background: Perishock pauses are pauses in chest compressions before and after defibrillatory shock. We examined the relationship between perishock pauses and survival to hospital discharge.
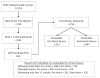
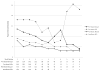
Methods and results: We included out-of-hospital cardiac arrest patients in the Resuscitation Outcomes Consortium Epistry-Cardiac Arrest who suffered arrest between December 2005 and June 2007, presented with a shockable rhythm (ventricular fibrillation or pulseless ventricular tachycardia), and had cardiopulmonary resuscitation process data for at least 1 shock (n=815). We used multivariable logistic regression to determine the association between survival and perishock pauses. In an analysis adjusted for Utstein predictors of survival, the odds of survival were significantly lower for patients with preshock pause ≥20 seconds (odds ratio, 0.47; 95% confidence interval, 0.27 to 0.82) and perishock pause ≥40 seconds (odds ratio, 0.54; 95% confidence interval, 0.31 to 0.97) compared with patients with preshock pause <10 seconds and perishock pause <20 seconds. Postshock pause was not independently associated with a significant change in the odds of survival. Log-linear modeling depicted a decrease in survival to hospital discharge of 18% and 14% for every 5-second increase in both preshock and perishock pause interval (up to 40 and 50 seconds, respectively), with no significant association noted with changes in the postshock pause interval.
Conclusions: In patients with cardiac arrest presenting in a shockable rhythm, longer perishock and preshock pauses were independently associated with a decrease in survival to hospital discharge. The impact of preshock pause on survival suggests that refinement of automatic defibrillator software and paramedic education to minimize preshock pause delays may have a significant impact on survival.
Figures
Comment in
-
ACP Journal Club. Longer perishock pauses were associated with decreased survival to hospital discharge after out-of-hospital shockable cardiac arrest.Ann Intern Med. 2011 Oct 18;155(8):JC4-12. doi: 10.7326/0003-4819-155-8-201110180-02012. Ann Intern Med. 2011. PMID: 22007071 No abstract available.
References
-
- Sans S, Kesteloot H, Kromhout D. Task Force of the European Society of Cardiology on Cardiovascular Morbidity and Mortality Statistics in Europe. The burden of cardiovascular diseases mortality in Europe. Eur Heart J. 1997;18:1231–1248. - PubMed
-
- Becker LB, Ostrander MP, Barret J, Kondos GT. Outcome of CPR in a large metropolitan area: where are the survivors? Ann Emerg Med. 1991;20:355–361. - PubMed
-
- Wik L, Kramer-Johansen J, Myklebust H, Sorebo H, Svensson L, Fellows B, Steen PA. Quality of cardiopulmonary resuscitation during out-of-hospital cardiac arrest. [see comment] JAMA. 2005;293:299–304. - PubMed
-
- Abella BS, Alvarado JP, Myklebust H, Edelson DP, Barry A, O’Hearn N, Vanden Hoek TL, Becker LB. Quality of cardiopulmonary resuscitation during in-hospital cardiac arrest.[see comment] JAMA. 2005;293:305–10. - PubMed
-
- Berg RA, Sanders AB, Kern KB, Hilwig RW, Heidenreich JW, Porter ME, Ewy GA. Adverse hemodynamic effects of interrupting chest compressions for rescue breathing during cardiopulmonary resuscitation for ventricular fibrillation cardiac arrest. Circulation. 200;104:2465–70. - PubMed
Publication types
MeSH terms
Grants and funding
- U01 HL077866/HL/NHLBI NIH HHS/United States
- U01 HL077865/HL/NHLBI NIH HHS/United States
- HL077867/HL/NHLBI NIH HHS/United States
- 5U01 HL077863/HL/NHLBI NIH HHS/United States
- HL077887/HL/NHLBI NIH HHS/United States
- U01 HL077881/HL/NHLBI NIH HHS/United States
- HL077873/HL/NHLBI NIH HHS/United States
- HL077871/HL/NHLBI NIH HHS/United States
- HL077881/HL/NHLBI NIH HHS/United States
- HL077908/HL/NHLBI NIH HHS/United States
- U01 HL077887/HL/NHLBI NIH HHS/United States
- U01 HL077885/HL/NHLBI NIH HHS/United States
- U01 HL077863/HL/NHLBI NIH HHS/United States
- U01 HL077908/HL/NHLBI NIH HHS/United States
- HL077872/HL/NHLBI NIH HHS/United States
- HL077866/HL/NHLBI NIH HHS/United States
- U01 HL077873/HL/NHLBI NIH HHS/United States
- U01 HL077867/HL/NHLBI NIH HHS/United States
- HL077885/HL/NHLBI NIH HHS/United States
- HL077865/HL/NHLBI NIH HHS/United States
- U01 HL077872/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

