Current pacemaker and defibrillator therapy
- PMID: 21691561
- PMCID: PMC3117174
- DOI: 10.3238/arztebl.2011.0372
Current pacemaker and defibrillator therapy
Abstract
Background: Pacemakers have been available for 50 years, and implantable cardiac defibrillators for 25. Clear indications for each have been established on the basis of data from randomized clinical trials (RCTs).
Methods: This review article is the product of a collaborative effort by a cardiologist and a cardiac surgeon. The authors arrived at a consensus through a selective review of the literature, with special attention to randomized controlled trials and registry data.
Results: Atrioventricular (AV) block only rarely necessitates permanent pacemaker stimulation after inferior myocardial infarction, of which it is a rare (12% to 20%) and often transient accompaniment. AV block is more common, however, in anterior wall infarction (frequency ca. 5%), and often necessitates permanent pacemaker therapy in such cases. Pacemaker complications are rare; they include oversensing (the detection of impulse noise) (0.7%), undersensing (the failure to detect impulses) (3.8%), electrode fractures (3.8%), isolation defects (3.4%), perforation (<1%), dislocation (<1%), and infection (<1% to 12%). Many RCTs have confirmed that defibrillators are effective in the prevention of sudden cardiac death (SCD): they lower the risk of SCD by 20% to 30% in primary prevention and by 20% to 40% in secondary prevention. Cardiac resynchronization therapy improves the clinical manifestations and outcome of patients with congestive heart failure, with a relative risk reduction (RR) of 20% to 40%, even among patients in NYHA classes I and II (RR ca. 40%). Implantable defibrillators only rarely cause problems or complications in either the short or the long term. Emotional disturbances, including anxiety, are a rare side effect, occurring in less than 1% of cases.
Conclusion: Pacemakers and implantable defibrillators are well-established electrotherapeutic devices that are highly effective and have only rare complications.
Figures
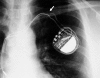

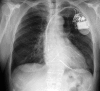
Comment in
-
Current pacemaker and defibrillator therapy. In the context of the end of life.Dtsch Arztebl Int. 2011 Oct;108(40):686; author reply 686. doi: 10.3238/arztebl.2011.0686a. Epub 2011 Oct 7. Dtsch Arztebl Int. 2011. PMID: 22114628 Free PMC article. No abstract available.
References
-
- Bayes de Luna A. Sudden death in ischemic heart disease. Rev Port Cardiol. 1990;9:473–479. - PubMed
-
- Ellenbogen KA, Wilkoff BL. Clinical cardiac pacing, defibrillation and resynchronization therapy. In: Lau CP, editor. 3rd edition. Philadelphia: Saunders Elsevier; 2006. pp. 1–1280.
-
- Lemke B, Nowak B, Pfeiffer D. Leitlinien zur Herzschrittmachertherapie. Z Kardiol. 2005;94:704–720. - PubMed
-
- Rybak K, Nowak B, Pfeiffer D, Fröhlich G, Lemke B. Kommentar zu den ESC-Leitlinien „Guidelines for cardiac pacing and cardiac resynchronization therapy“. Kardiologe. 2008;2:463–478.
-
- Wellens HJJ, Conover B. The ECG in acute ST-segment elevation MI. In: Wellens HJJ, Conover B, editors. The ECG in emergency decision making. 2nd edition. St. Louis: WB Saunders Company; 2006. pp. 1–53.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

