Intra-arterial therapy for acute ischemic stroke
- PMID: 21717263
- PMCID: PMC3250276
- DOI: 10.1007/s13311-011-0059-8
Intra-arterial therapy for acute ischemic stroke
Abstract
Intra-arterial therapy (IAT) for acute ischemic stroke refers to endovascular catheter-based approaches to achieve recanalization using mechanical clot disruption, locally injected thrombolytic agents or both. IAT may be used in addition to intravenous tissue plasminogen activator (tPA) or in patients who do not qualify for tPA, usually because they are outside the approved 3-h timeframe window or have contraindications, such as elevated international normalized ratio or partial thromboplastin time. Recanalization rates correlate with clinical improvement, and with the newest catheters it is possible to achieve recanalization in roughly 80% of patients treated. However, while the catheters are approved by the Food and Drug Administration, there are still no randomized trial data demonstrating the role of current IAT therapy vs either tPA or standard management. IAT is reserved for patients with large artery occlusions in the basilar, distal carotid, or proximal middle cerebral arteries. Imaging the penumbra using magnetic resonance imaging or computed tomographic perfusion is currently the most frequently used way to identify patients who might benefit. However, the imaging and clinical criteria for identifying which patients benefit, and perhaps more importantly those who will do poorly despite IAT, remain unclear.
Figures
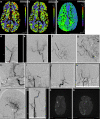

References
-
- Saqqur M, Uchino K, Demchuk AM, et al. Site of arterial occlusion identified by transcranial Doppler predicts the response to intravenous thrombolysis for stroke. Stroke. 2007;38:948–954. doi: 10.1161/01.STR.0000257304.21967.ba. - DOI - PubMed
-
- Boer SP, Barnes EH, Westerhout CM, et al. High-risk patients with ST-elevation myocardial infarction derive greatest absolute benefit from primary percutaneous coronary intervention: results from the Primary Coronary Angioplasty Trialist versus thrombolysis (PCAT)-2 collaboration. Am Heart J. 2011;161:500–507. doi: 10.1016/j.ahj.2010.11.022. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

