Allopurinol benefits left ventricular mass and endothelial dysfunction in chronic kidney disease
- PMID: 21719783
- PMCID: PMC3137586
- DOI: 10.1681/ASN.2010111185
Allopurinol benefits left ventricular mass and endothelial dysfunction in chronic kidney disease
Abstract
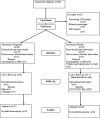
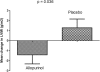
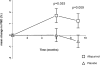
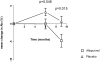
Allopurinol ameliorates endothelial dysfunction and arterial stiffness among patients without chronic kidney disease (CKD), but it is unknown if it has similar effects among patients with CKD. Furthermore, because arterial stiffness increases left ventricular afterload, any allopurinol-induced improvement in arterial compliance might also regress left ventricular hypertrophy (LVH). We conducted a randomized, double-blind, placebo-controlled, parallel-group study in patients with stage 3 CKD and LVH. We randomly assigned 67 subjects to allopurinol at 300 mg/d or placebo for 9 months; 53 patients completed the study. We measured left ventricular mass index (LVMI) with cardiac magnetic resonance imaging (MRI), assessed endothelial function by flow-mediated dilation (FMD) of the brachial artery, and evaluated central arterial stiffness by pulse-wave analysis. Allopurinol significantly reduced LVH (P=0.036), improved endothelial function (P=0.009), and improved the central augmentation index (P=0.015). This study demonstrates that allopurinol can regress left ventricular mass and improve endothelial function among patients with CKD. Because LVH and endothelial dysfunction associate with prognosis, these results call for further trials to examine whether allopurinol reduces cardiovascular events in patients with CKD and LVH.
Copyright © 2011 by the American Society of Nephrology
Figures
Comment in
-
Cardiovascular disease: Allopurinol reduces left ventricular hypertrophy.Nat Rev Nephrol. 2011 Aug 2;7(9):487. doi: 10.1038/nrneph.2011.100. Nat Rev Nephrol. 2011. PMID: 21808279 No abstract available.
References
-
- Foley RN, Parfrey PS, Sarnak MJ: Clinical epidemiology of cardiovascular disease in chronic renal disease. Am J Kidney Dis 32[5 Suppl 3]: S112–S119, 1998 - PubMed
-
- Wanner C, Krane V, Marz W, Olschewski M, Mann JF, Ruf G, Ritz E: Atorvastatin in patients with type 2 diabetes mellitus undergoing hemodialysis. N Engl J Med 353: 238–248, 2005 - PubMed
-
- Fellstrom BC, Jardine AG, Schmieder RE, Holdaas H, Bannister K, Beutler J, Chae DW, Chevaile A, Cobbe SM, Gronhagen-Riska C, De Lima JJ, Lins R, Mayer G, McMahon AW, Parving HH, Remuzzi G, Samuelsson O, Sonkodi S, Sci D, Suleymanlar G, Tsakiris D, Tesar V, Todorov V, Wiecek A, Wuthrich RP, Gottlow M, Johnsson E, Zannad F: Rosuvastatin and cardiovascular events in patients undergoing hemodialysis. N Engl J Med 360: 1395–1407, 2009 - PubMed
-
- Sharp Collaborative Group: Study of Heart and Renal Protection (SHARP): Randomized trial to assess the effects of lowering low-density lipoprotein cholesterol among 9,438 patients with chronic kidney disease. Am Heart J 160: 785–794.e710, 2010 - PubMed
-
- Butler R, Morris AD, Belch JJ, Hill A, Struthers AD: Allopurinol normalizes endothelial dysfunction in type 2 diabetics with mild hypertension. Hypertension 35: 746–751, 2000 - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

