Beam angle manipulation to reduce cardiac dose during breast radiotherapy
- PMID: 21750129
- PMCID: PMC3473992
- DOI: 10.1259/bjr/58636261
Beam angle manipulation to reduce cardiac dose during breast radiotherapy
Abstract
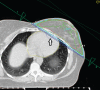
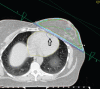
Objective: Standard tangential radiotherapy techniques after breast conservative surgery (BCS) often results in the irradiation of the tip of the left ventricle and the left anterior descending coronary artery (LAD), potentially increasing cardiovascular morbidity. The importance of minimising radiation dose to these structures has attracted increased interest in recent years. We tested a hypothesis that in some cases, by manipulating beam angles and accepting lower-than-prescribed doses of radiation in small parts of the breast distant from the surgical excision site, significant cardiac sparing can be achieved compared with more standard plans.
Methods: A sample of 12 consecutive patients undergoing radiotherapy after left-sided BCS was studied. All patients were planned with a 6 MV tangential beam, beam angles were manipulated carefully and if necessary lower doses were given to small parts of the breast distant from the surgical excision site to minimise cardiac irradiation ("institutional" plan). Separate "hypothetical standard" plans were generated for seven patients using set field margins that met published guidelines.
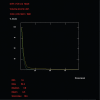
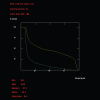
Results: In seven patients, the institutional plans resulted in lower doses to the LAD and myocardium than the hypothetical standard plans. In the other five patients, LAD and myocardial doses were deemed minimal using the hypothetical standard plan, which in these patients corresponded to the institutional plan (the patients were actually treated using the institutional plans).
Conclusion: Much attention has been devoted to ways of minimising cardiac radiation dose. This small sample demonstrates that careful manipulation of beam angles can often be a simple, but effective technique to achieve this.
Figures

References
-
- Westlake S, Cooper N.Office for National Statistics. Cancer incidence and mortality: trends in the United Kingdom and constituent countries, 1993 to 2004. [cited 8 November 2010] Available from: http://www.nos.gov.uk/ons/rel/hsq/health-statistics-quarterly/no--38--su.... - PubMed
-
- Lichter AS, Lippman ME, Danforth DN, d'Angelo T, Steinberg SM, deMoss E, et al. Mastectomy versus breast-conserving therapy in the treatment of stage I and II carcinoma of the breast: A randomized trial at the National Cancer Institute. J Clin Oncol 1992;10:976–83 - PubMed
-
- Van Dongen JA, Voogd AC, Fentiman IS, Legrand C, Sylvester RJ, Tong D, et al. Long-term results of a randomized trial comparing breast-conserving therapy with mastectomy: European Organization for Research and Treatment of Cancer 10801 trial. J Natl Cancer Inst 2000;92:1143–50 - PubMed
-
- Fisher B, Anderson S, Bryant J, Margolese RG, Deutsch M, Fisher ER, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med 2002;347:1233–41 - PubMed
-
- Taylor CW, Nisbet A, McGale P, Darby SC. Cardiac exposures in breast cancer radiotherapy: 1950s–1990s. Int J Radiat Oncol Biol Phys 2007;69:1484–95 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

