Functional capacity of Mycobacterium tuberculosis-specific T cell responses in humans is associated with mycobacterial load
- PMID: 21775682
- PMCID: PMC3159795
- DOI: 10.4049/jimmunol.1101122
Functional capacity of Mycobacterium tuberculosis-specific T cell responses in humans is associated with mycobacterial load
Abstract
High Ag load in chronic viral infections has been associated with impairment of Ag-specific T cell responses; however, the relationship between Ag load in chronic Mycobacterium tuberculosis infection and functional capacity of M. tuberculosis-specific T cells in humans is not clear. We compared M. tuberculosis-specific T cell-associated cytokine production and proliferative capacity in peripheral blood from adults with progressively higher mycobacterial loads-that is, persons with latent M. tuberculosis infection (LTBI), with smear-negative pulmonary tuberculosis (TB), and smear-positive TB. Patients with smear-positive TB had decreased polyfunctional IFN-γ(+)IL-2(+)TNF-α(+) and IL-2-producing specific CD4 T cells and increased TNF-α single-positive cells, when compared with smear-negative TB and LTBI. TB patients also had increased frequencies of M. tuberculosis-specific CD8 T cells, compared with LTBI. M. tuberculosis-specific CD4 and CD8 T cell proliferative capacity was profoundly impaired in individuals with smear-positive TB, and correlated positively with ex vivo IFN-γ(+)IL-2(+)TNF-α(+) CD4 T cells, and inversely with TNF-α single-positive CD4 T cells. During 6 mo of anti-TB treatment, specific IFN-γ(+)IL-2(+)TNF-α(+) CD4 and CD8 T cells increased, whereas TNF-α and IFN-γ single-positive T cells decreased. These results suggest progressive impairment of M. tuberculosis-specific T cell responses with increasing mycobacterial load and recovery of responses during therapy. Furthermore, these data provide a link between specific cytokine-producing subsets and functional capacity of M. tuberculosis-specific T cells, and between the presence of specific CD8 T cells ex vivo and active TB disease. These data have potentially significant applications for the diagnosis of TB and for the identification of T cell correlates of TB disease progression.
Figures
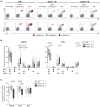





References
-
- Global Tuberculosis Control. World Health Organization; 2010.
-
- Caruso AM, Serbina N, Klein E, Triebold K, Bloom BR, Flynn JL. Mice deficient in CD4 T cells have only transiently diminished levels of IFN-gamma, yet succumb to tuberculosis. J Immunol. 1999;162:5407–5416. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

