Cellular immune responses to nine Mycobacterium tuberculosis vaccine candidates following intranasal vaccination
- PMID: 21799939
- PMCID: PMC3143185
- DOI: 10.1371/journal.pone.0022718
Cellular immune responses to nine Mycobacterium tuberculosis vaccine candidates following intranasal vaccination
Abstract
Background: The identification of Mycobacterium tuberculosis vaccines that elicit a protective immune response in the lungs is important for the development of an effective vaccine against tuberculosis.
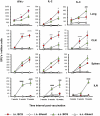
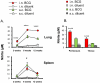
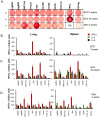
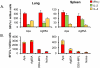
Methods and principal findings: In this study, a comparison of intranasal (i.n.) and subcutaneous (s.c.) vaccination with the BCG vaccine demonstrated that a single moderate dose delivered intranasally induced a stronger and sustained M. tuberculosis-specific T-cell response in lung parenchyma and cervical lymph nodes of BALB/c mice than vaccine delivered subcutaneously. Both BCG and a multicomponent subunit vaccine composed of nine M. tuberculosis recombinant proteins induced strong antigen-specific T-cell responses in various local and peripheral immune compartments. Among the nine recombinant proteins evaluated, the alanine proline rich antigen (Apa, Rv1860) was highly antigenic following i.n. BCG and immunogenic after vaccination with a combination of the nine recombinant antigens. The Apa-induced responses included induction of both type 1 and type 2 cytokines in the lungs as evaluated by ELISPOT and a multiplexed microsphere-based cytokine immunoassay. Of importance, i.n. subunit vaccination with Apa imparted significant protection in the lungs and spleen of mice against M. tuberculosis challenge. Despite observed differences in the frequencies and location of specific cytokine secreting T cells both BCG vaccination routes afforded comparable levels of protection in our study.
Conclusion and significance: Overall, our findings support consideration and further evaluation of an intranasally targeted Apa-based vaccine to prevent tuberculosis.
Conflict of interest statement
Figures


References
-
- Dye C, Williams BG. The population dynamics and control of tuberculosis. Science. 2010;328:856–861. - PubMed
-
- Andersen P, Doherty TM. The success and failure of BCG - implications for a novel tuberculosis vaccine. Nat Rev Microbiol. 2005;3:656–662. - PubMed
-
- Kaufmann SH. Future vaccination strategies against tuberculosis: thinking outside the box. Immunity. 2010;33:567–577. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

