Acceptance and tolerability of an adjuvanted nH1N1 vaccine in HIV-infected patients in the Cologne-Bonn cohort
- PMID: 21813369
- PMCID: PMC3352000
- DOI: 10.1186/2047-783x-16-7-289
Acceptance and tolerability of an adjuvanted nH1N1 vaccine in HIV-infected patients in the Cologne-Bonn cohort
Abstract
Objective: To evaluate the acceptance and tolerability of the nH1N1 2009 vaccine in HIV-positive individuals.
Method: 758 patients were included in this prospective study. Different study populations were formed: The Tolerability Study Group consists of HIV-infected patients who visited three outpatient clinics (Cologne, Bonn, Freiburg) during a predefined time period. Patients were offered nH1N1 vaccination. Those accepting were administered a standard dose AS03 adjuvant nH1N1 vaccine. Questionnaires to report side effects occurring within 7 days after immunization were handed out. In a substudy conducted during the same time period, acceptance towards immunization was recorded. This Acceptance Study Group consists of all HIV-infected patients visiting the Cologne clinic. They were offered vaccination. In case of refusal, motivation was recorded.
Results: In the Tolerability Study Group, a total of 475 patient diaries returned in the three study centres could be evaluated, 119 of those (25%) reported no side effects. Distribution of symptoms was as follows: Pain 285/475 patients (60%), swelling 96 (20%), redness 54 (11%), fever 48/475 (10%), muscle/joint ache 173 (36%), headache 127 (27%), and fatigue 210 (44%). Association of side effects with clinical data was calculated for patients in Cologne and Bonn. Incidence of side effects was significantly associated with CDC stages A, B compared to C, and with a detectable viral load (>50 copies/mL). No correlation was noted for CD4 cell count, age, gender or ethnicity. - In the Acceptance Study Group, 538 HIV-infected patients were offered vaccination, 402 (75%) accepted, while 136 (25%) rejected. Main reasons for rejection were: Negative media coverage (35%), indecisiveness with preference to wait until a later date (23%), influenza not seen as personal threat (19%) and scepticism towards immunization in general (10%).
Conclusion: A total of 622 HIV-infected patients were vaccinated against nH1N1-influenza in the three study centres. No severe adverse events were reported. The tolerability was in most parts comparable to general population. Acceptance rate towards influenza vaccination was high (75%). Those refusing the immunization mentioned negative media coverage as the major influence on their decision.
Figures

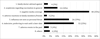
Similar articles
-
Responses to pandemic ASO3-adjuvanted A/California/07/09 H1N1 influenza vaccine in human immunodeficiency virus-infected individuals.BMC Immunol. 2012 Aug 31;13:49. doi: 10.1186/1471-2172-13-49. BMC Immunol. 2012. PMID: 22937824 Free PMC article.
-
Open-label, randomised, parallel-group, multicentre study to evaluate the safety, tolerability and immunogenicity of an AS03(B)/oil-in-water emulsion-adjuvanted (AS03(B)) split-virion versus non-adjuvanted whole-virion H1N1 influenza vaccine in UK children 6 months to 12 years of age.Health Technol Assess. 2010 Oct;14(46):1-130. doi: 10.3310/hta14460-01. Health Technol Assess. 2010. PMID: 20923610 Clinical Trial.
-
[Attitudes and side effects related to pandemic influenza A (H1N1) vaccination in healthcare personnel].Mikrobiyol Bul. 2012 Jan;46(1):57-64. Mikrobiyol Bul. 2012. PMID: 22399172 Turkish.
-
Adjuvanted-influenza vaccination in patients infected with HIV: a systematic review and meta-analysis of immunogenicity and safety.Hum Vaccin Immunother. 2020 Mar 3;16(3):612-622. doi: 10.1080/21645515.2019.1672492. Epub 2019 Nov 1. Hum Vaccin Immunother. 2020. PMID: 31567058 Free PMC article.
-
Narcolepsy, 2009 A(H1N1) pandemic influenza, and pandemic influenza vaccinations: what is known and unknown about the neurological disorder, the role for autoimmunity, and vaccine adjuvants.J Autoimmun. 2014 May;50:1-11. doi: 10.1016/j.jaut.2014.01.033. Epub 2014 Feb 19. J Autoimmun. 2014. PMID: 24559657 Review.
References
-
- Dawood FS, Jain S, Finelli L, Shaw MW, Lindstrom S, Garten RJ, Gubareva LV, Xu X, Bridges CB, Uyeki TM. Emergence of a novel swine-origin influenza A (H1N1) virus in humans. N Engl J Med. 2009;360(25):2605–15. - PubMed
-
- team NiAHNi. Description of the early stage of pandemic (H1N1) 2009 in Germany, 27 April-16 June 2009. Euro Surveill. 2009;14(31) - PubMed
-
- Gilsdorf A, Poggensee G. Influenza A(H1N1)v in Germany: the first 10,000 cases. Euro Surveill. 2009;14(34) - PubMed
-
- RKI RKI. Zur aktuellen Situation bei ARE/Influenza für die 39. Kalenderwoche 2009. Epid Bull. 2009. p. 1.
-
- Johansen K, Nicoll A, Ciancio BC, Kramarz P. Pandemic influenza A(H1N1) 2009 vaccines in the European Union. Euro Surveill. 2009;14(41):19361. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

