Dialysate sodium, serum sodium and mortality in maintenance hemodialysis
- PMID: 21891777
- PMCID: PMC3471551
- DOI: 10.1093/ndt/gfr497
Dialysate sodium, serum sodium and mortality in maintenance hemodialysis
Abstract
Background: Individuals with end-stage kidney disease appear to have stable pre-dialysis serum sodium concentrations over time, with lower values associating with increased mortality. Dialysate sodium concentrations have increased over many years in response to shorter treatments, but the relationship between serum sodium, dialysate sodium and outcomes in chronic hemodialysis patients has not yet been systematically examined.
Methods: We studied a cohort of 2272 individuals receiving thrice-weekly hemodialysis treatment. Available data included demographics, laboratory and clinical measures, details of the dialysis prescription and 30-month follow-up. We examined the distribution of serum and dialysate sodium among subjects and compared mortality according to dialysate and serum sodium concentrations using Cox regression models.
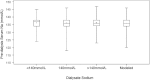
Results: Dialysate sodium concentration varied within and among dialysis centers. The pre-dialysis serum sodium concentration (mean 136.1 mmol/L) did not differ across dialysate sodium concentrations. There was evidence for effect modification for mortality according to differing serum sodium and dialysate sodium concentrations (P=0.05). For each 4 mmol/L increment in serum sodium, the hazard ratio for death was 0.72 [95% confidence interval (CI) 0.63-0.81] with lower dialysate sodium compared to 0.86 (95% CI 0.75-0.99) for higher dialysate sodium. Higher dialysate sodium concentration was associated with mortality at higher, but not lower, pre-dialysis serum sodium concentrations.
Conclusions: The pre-dialysis serum sodium concentration appears to be unaffected by the dialysate sodium concentration. The relationship between serum and dialysate sodium and mortality appears to be variable. Further research is warranted to determine the biological mechanisms of these associations and to re-examine total body sodium handling in hemodialysis.
Figures



References
-
- Flanigan MJ. Role of sodium in hemodialysis. Kidney Int Suppl. 2000;76:S72–S78. - PubMed
-
- Peixoto AJ, Gowda N, Parikh CR, et al. Long-term stability of serum sodium in hemodialysis patients. Blood Purif. 2010;29:264–267. - PubMed
-
- Keen ML, Gotch FA. The association of the sodium “setpoint” to interdialytic weight gain and blood pressure in hemodialysis patients. Int J Artif Organs. 2007;30:971–979. - PubMed
-
- Lambie SH, Taal MW, Fluck RJ, et al. Online conductivity monitoring: validation and usefulness in a clinical trial of reduced dialysate conductivity. ASAIO J. 2005;51:70–76. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

