Comparative study of intravenously administered clonidine and magnesium sulfate on hemodynamic responses during laparoscopic cholecystectomy
- PMID: 21897505
- PMCID: PMC3161459
- DOI: 10.4103/0970-9185.83679
Comparative study of intravenously administered clonidine and magnesium sulfate on hemodynamic responses during laparoscopic cholecystectomy
Abstract
Background: Both magnesium and clonidine are known to inhibit catecholamine and vasopressin release and attenuate hemodynamic response to pneumoperitoneum. This randomized, double blinded, placebo controlled study has been designed to assess which agent attenuates hemodynamic stress response to pneumoperitoneum better.
Materials and methods: 120 patients undergoing elective laparoscopic cholecystectomy were randomized into 4 groups of 30 each. Group K patients received 50 ml normal saline over a period of 15 min after induction and before pneumoperitoneum, group M patients received 50 mg/kg of magnesium sulfate in normal saline (total volume 50 ml) over same time duration. Similarly group C1 patients received 1 μg/kg clonidine and group C2 1.5 μg/kg clonidine respectively in normal saline (total volume 50 ml). Blood pressure and heart rate were recorded before induction (baseline value), at the end of infusions and every 5 min after pneumoperitoneum.
Statistical analysis: Paired t test was used for intra-group comparison and ANOVA for inter-group comparison.
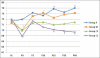
Results: Systolic blood pressure was significantly higher in control group as compared to all other groups during pneumoperitoneum. On comparing patients in group M and group C1, no significant difference in systolic BP was found at any time interval. Patients in group C2 showed best control of systolic BP. As compared to group M and group C1, BP was significantly lower at 10, 30 and 40 min post pneumoperitoneum. No significant episodes of hypotension were found in any of the groups. Extubation time and time to response to verbal command like eye opening was significantly longer in group M as compared to other groups.
Conclusion: Administration of magnesium sulfate or clonidine attenuates hemodynamic response to pneumoperitoneum. Although magnesium sulfate 50 mg/kg produces hemodynamic stability comparable to clonidine 1 μg/kg, clonidine in doses of 1.5μg/kg blunts the hemodynamic response to pneumoperitoneum more effectively.
Keywords: Clonidine; laparoscopic cholecystectomy; magnesium sulfate; pneumoperitoneum.
Conflict of interest statement
Figures

References
-
- Joris JL, Chiche JD, Canivet JL, Jacquet NJ, Legros JJ, Lamy ML. Haemodynamic changes induced by laparoscopy and their endocrine correlates: Effects of clonidine. J Am Coll Cardiol. 1998;32:1389–96. - PubMed
-
- Wabha RW, Beique F, Kleiman SJ. Cardiopulmonary function and laparoscopic cholecystectomy. Can J Anaesth. 1995;42:51–63. - PubMed
-
- Sharma KC, Brandstetter RD, Brensilver JM, Jung LD. Cardiopulmonary physiology and pathophysiology as a consequence of laparoscopic surgery. Chest. 1996;110:810–5. - PubMed
-
- Mikami O, Kawakita S, Fujise K, Shingu K, Takahashi H, Matsuda T. Catecholamine release caused by carbondioxide insufflation during laparoscopic surgery. J Urol. 1996;155:1368–71. - PubMed
-
- Myre K, Rostrup M, Buanes T, Stokland O. Plasma catecholamines and haemodynamic changes during pneumoperitoneum. Acta Anaesthesiol Scand. 1998;42:343–7. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

