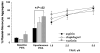Circulating inflammatory cells are associated with vein graft stenosis
- PMID: 21906902
- PMCID: PMC3538859
- DOI: 10.1016/j.jvs.2011.04.039
Circulating inflammatory cells are associated with vein graft stenosis
Abstract
Objective: Infrainguinal autogenous vein grafts are especially prone to narrowing and failure, and both inflammatory and thrombotic pathways are implicated. Platelets and monocytes are the key thrombo-inflammatory cells that arrive first at sites of vascular injury. These cells have potent interactions that recruit and activate one another, propagating thrombotic and inflammatory responses within the vessel wall. We therefore hypothesized that elevated levels of platelet-monocyte aggregates (PMA) might be associated with stenosis, and could possibly discriminate between patients with or without vein graft stenosis.
Methods: Thirty-six vascular surgery patients were studied, in a stable quiescent period after infrainguinal autogenous vein graft bypasses for occlusive disease. Eighteen patients had hemodynamically significant graft stenoses confirmed by imaging, and 18 were free from stenosis. The level of PMA in whole blood was quantified after blood draw using two-color flow cytometry. Three measurements were made per sample: the basal, in-vivo level of aggregates (baseline PMA); the predisposition to spontaneously generate PMA (spontaneous PMA); and PMA generation by the addition of exogenous thrombin receptor-activating peptide (stimulated PMA). The baseline, in-vivo level of PMA was estimated by immediate flow analysis. The predisposition to spontaneously generate PMA was measured after in vitro incubation. Responsiveness to thrombin stimulation of the blood was quantified by the in vitro dose response to an exogenous thrombin receptor-activating peptide (sfllrn).
Results: Baseline PMA levels were similar in patients with vein graft stenosis vs nonstenosis (14.8% ± 3.2 vs 10.1% ± 1.5, respectively, mean ± SEM). However, patients with stenosis showed higher spontaneous PMA levels (58.5% ± 4.5 vs 28.3% ± 4.3; P < .001) and higher stimulated PMA levels (P < .001; analysis of variance). Covariables of smoking, diabetes, statin, or antithrombotic therapy could not account for these differences.
Conclusions: Platelet-monocyte reactivity may play a role in the development of vein graft stenoses. Those with/without stenosis differed primarily in their threshold, or predisposition to form aggregates (spontaneous PMA), while their basal circulating levels of PMA (baseline PMA) were similar. These measurements may unmask pathologic differences in thrombo-inflammatory responsiveness that are not apparent in basal measurements. Understanding the causes and mechanisms leading to abnormal platelet-monocyte responses may improve approaches to predicting or preventing vein graft stenosis.
Copyright © 2011 Society for Vascular Surgery. All rights reserved.
References
-
- Mills JL, Wixon CL, James DCM, Devine J, Westerband A, Hughes JD. The natural history of intermediate and critical vein graft stenosis: Recommendations for continued surveillance or repair. J Vasc Surg. 2001;33:273–80. - PubMed
-
- Gupta AK, Bandyk DF, Cheanvechai D, Johnson BL. Natural history of infrainguinal vein graft stenosis relative to bypass grafting technique. J Vasc Surg. 1997;25(2):211–20. - PubMed
-
- Visser K, Idu MM, Buth J, Engel GL, Hunink MG. Duplex scan surveillance during the first year after infrainguinal autologous vein bypass grafting surgery: costs and clinical outcomes compared with other surveillance programs. J Vasc Surg. 2001;33(1):123–30. - PubMed
-
- Conte MS, Bandyk DF, Clowes AW, Moneta GL, Seely L, Lorenz TJ, et al. Results of PREVENT III: a multicenter, randomized trial of edifoligide for the prevention of vein graft failure in lower extremity bypass surgery. J Vasc Surg. 2006;43(4):742–51. - PubMed
-
- Conte MS. Technical factors in lower-extremity vein bypass surgery: How can we improve outcomes? Semin Vasc Surg. 2009;22:227–33. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical